Preventing back injuries to nursing staff is one of the most important things we can do in healthcare and starts with reducing overexertion and modifying predictable manual patient handling tasks like Lateral Transfers and repositioning patients in bed.
Lateral Transfers and The Risks
Lateral transfers have been identified as some of the riskiest tasks in handling of patients in hospitals because patients may be moved from one surface to another several times in a day, and this is mostly done manually. Many healthcare workers are prone to musculoskeletal disorders resulting from manual transfer of patients since the task may be carried out by a few workers which results in having to strain. The equipment used in manual transfer of patients does not have the necessary designs for minimizing friction, and this contributes to increased risk of injury to both healthcare workers and the patients. A repositioning injury could also occur when the nurses are trying to change the position of a patient on the bed or moving them to a different surface.
A recent study found that the prevalence of musculoskeletal disorders and more specifically lower back pains was around 55 percent for nurses and nurse aides annually. Another study involving 22 hospitals and at least 100 clinics with a cumulative of 33000 healthcare workers found that an average of 205 workers experienced some injuries per year, and the average cost of treatment was 1.5 million dollars each year. Manual patient handling is associated with numerous types of injuries such as back pains, shoulder, neck, and wrist injuries among other injuries that could result in permanent disability which makes it unsafe.
Different States have enacted safe patient handling laws that require the use of transfer aids, assistive devices, and engineering controls in the lifting of patients to replace manual tasks of moving patients. These laws are meant to keep both patients and the healthcare workers safe from the common injuries associated with manual transfers. In Washington State, for example, hospitals are required to obtain lifting equipment for the purpose of patient handling, and they are given tax credits for this equipment. Still in the State of Washington, a healthcare worker is allowed to refuse to engage in patient handling activity when the worker believes that the activity may expose the patient or a healthcare worker to an unacceptable risk of getting injured.
Air Powered Patient Transfer Devices Helping Nurses and Back Injuries
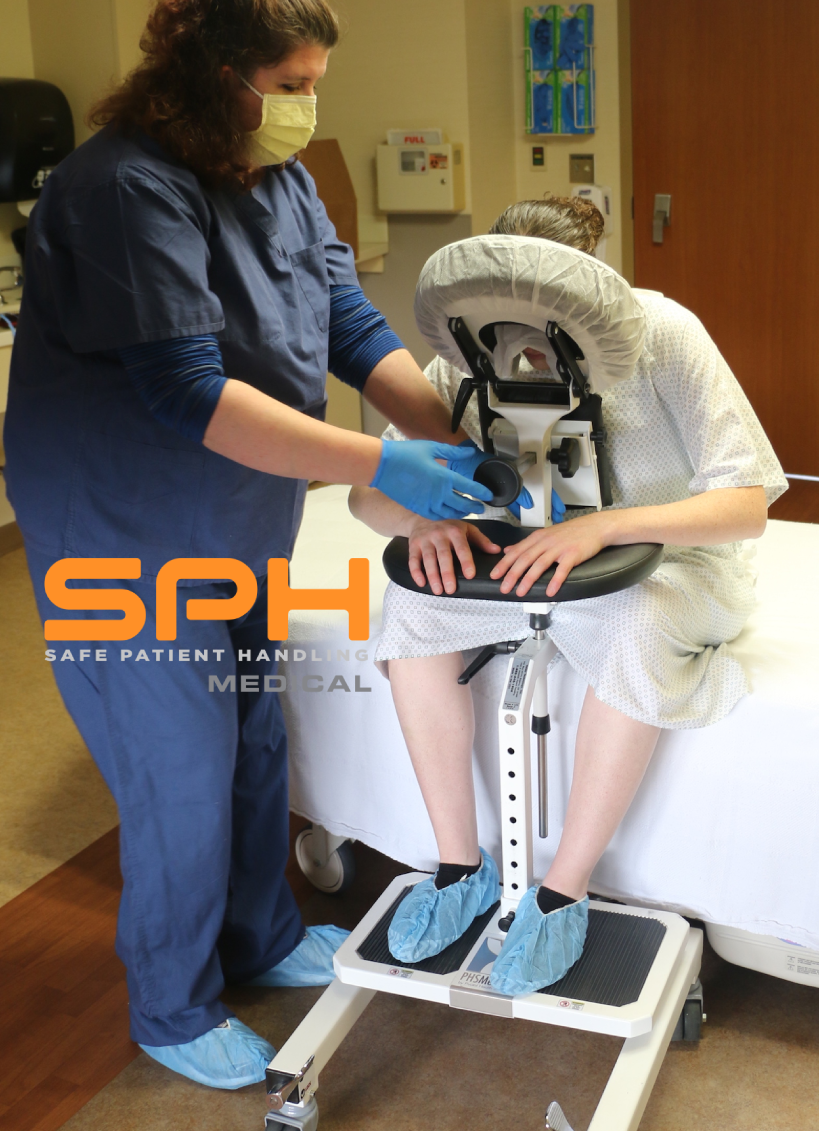
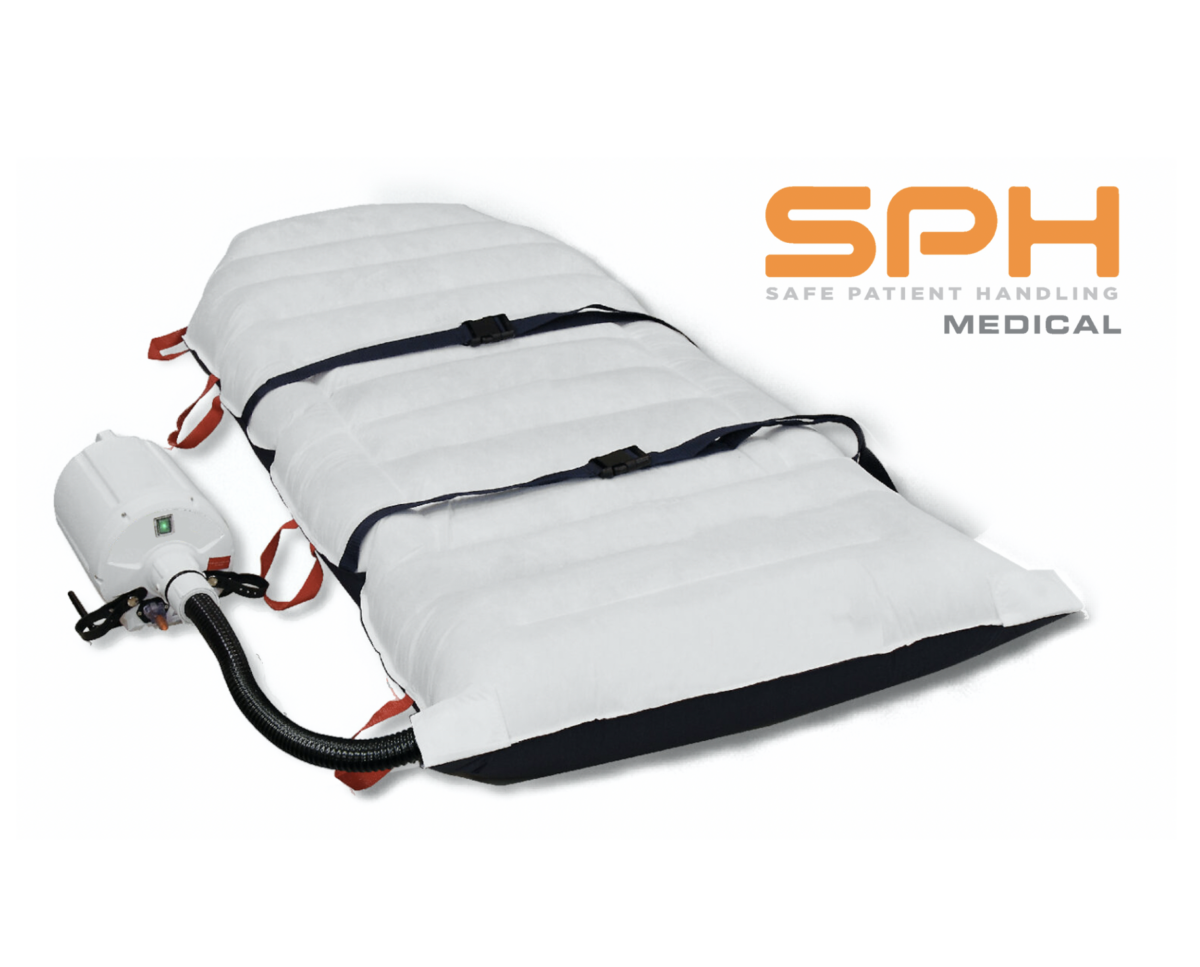
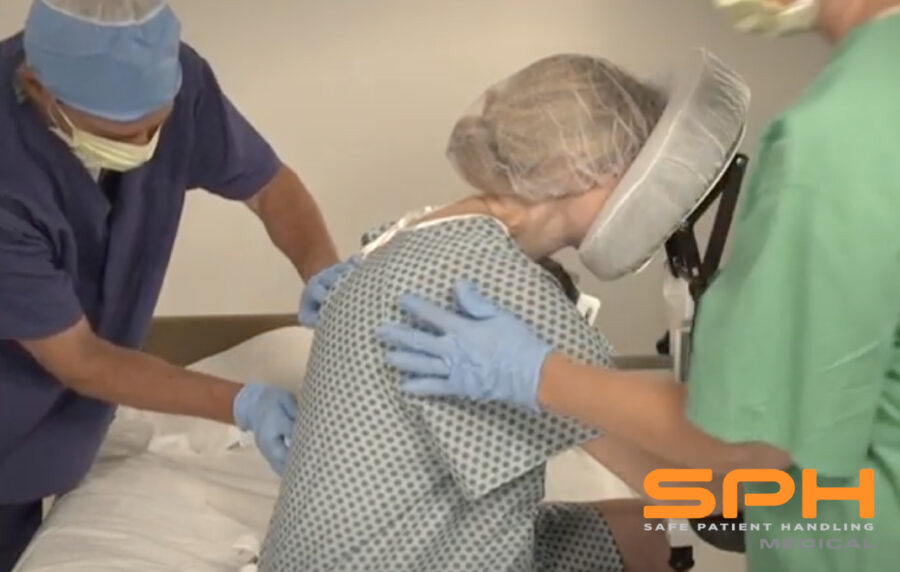
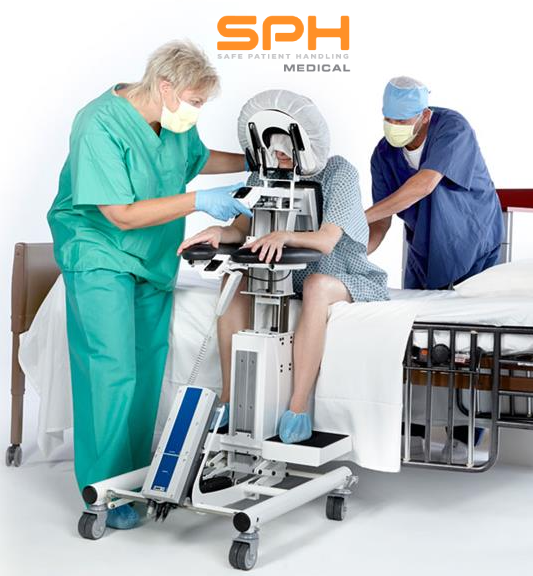
The evidence-based safe patient handling procedures emphasize the appropriate use of lifting equipment and assistive devices to make it easier and safer for both nurses and patients during the transfer process. Some of the most popular assistive devices include the Air Powered Patient Transfer Devices like SPH Medical’s Air Transfer System or Hovermatt and AirPal which are designed to reduce friction and simplify the task of repositioning a patient from one surface to another. These Air Powered transfer devices help in minimizing the risk of a repositioning injury and other nursing injury because they are placed underneath a patient and then inflated whenever the patient needs to be repositioned on the bed. Air Powered lateral transfer systems have been designed to release air through the bottom of the mattress surface to create a thin layer of air that reduces the amount of friction during the task of boosting or moving a patient and to evenly distribute pressure.
AirPowered lateral transfer systems have numerous benefits to healthcare workers and the patients including increased comfort. This is because the air transfer devices eliminate the grabbing and pulling from manual transfer methods. In addition the patient’s weight is evenly redistributed in a balanced way to ensure that the patient feels much more comfortable and safe. For patients who are quite heavy, the Air Powered transfer devices provide a sense of dignity to patients of size because they allow fewer people to handle them safely. With the air flow significantly reducing friction a morbidly obese patient or patient of size can be moved with relative ease. Fewer nurses having to assist means that the patient doesn’t have to feel embarrassed about their weight. The devices also make it safer for patients compared to the manual transfer devices by reducing friction and other factors that cause patients to slip and fall when being moved. Some special features are incorporated in the Air Powered lateral transfer systems to increase the safety of patients and nurses such as safety straps for securing the patient during the transfer process.
Many studies have observed that the risk of nursing injury is greatly reduced in hospitals where Air Transfer Systems have been deployed. The fact that most States have enacted safe patient handling laws that demand hospitals to acquire and implement lifting equipment and assistive devices shows that these devices are important in ensuring the safety of patients, nurses, and other stakeholders in the healthcare industry. Where the hospitals are required to have these devices, purchasing reputable brands not only ensures that they remain compliant with the State’s regulations but also they guarantee the well-being of their employees and patients. As noted above, hundreds of injuries occur due to manual transfers, and these injuries require millions of dollars to treat. These costs and other undesirable consequences can be minimized or eliminated by the use of Air Powered transfer devices since they are specifically designed to eliminate the risks associated with handling patients.
Contact SPH Medical to learn more about Air Transfer Technology and begin to reduce injuries in your hospital or healthcare facility.