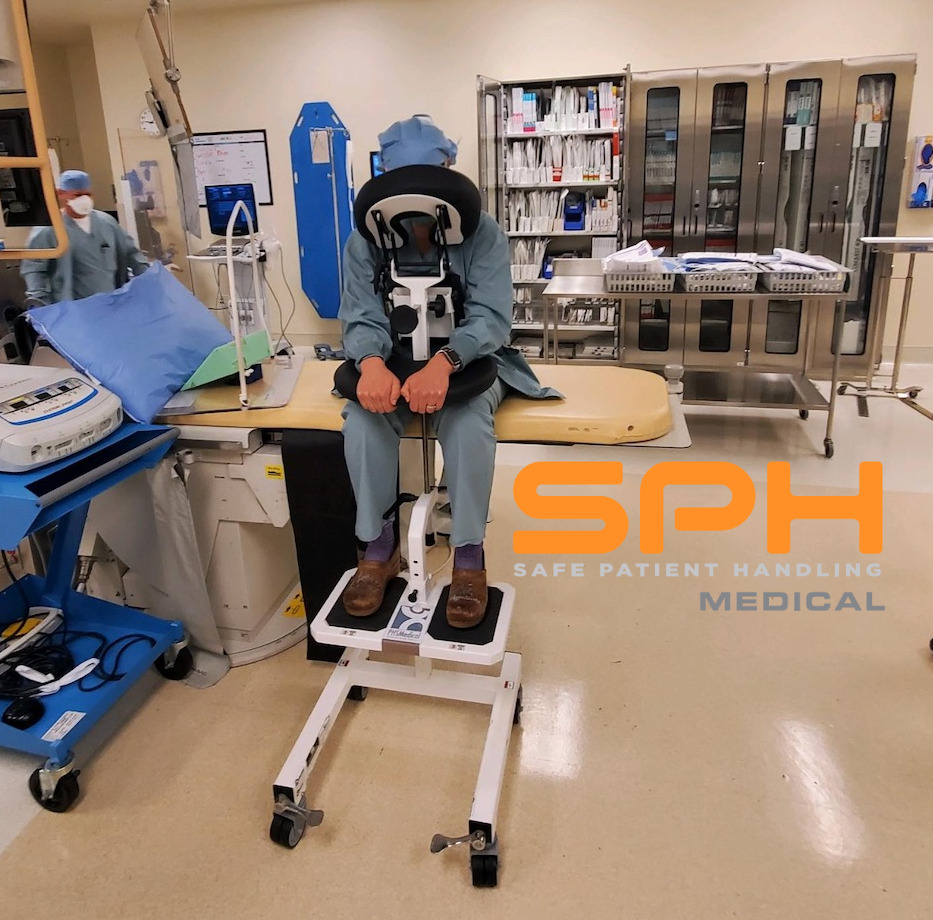
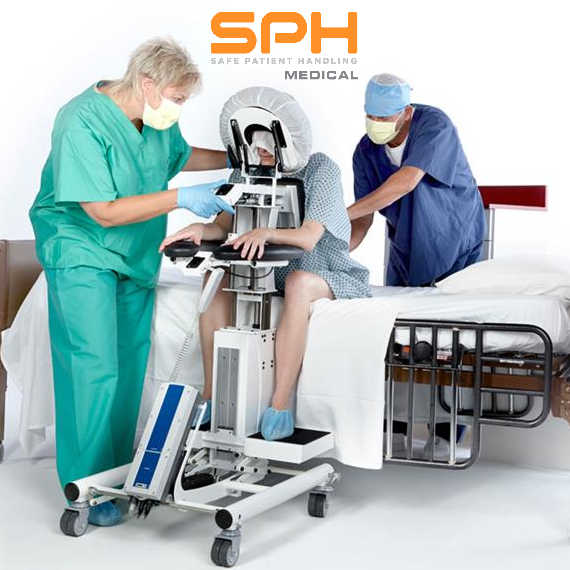
The EPD improves surgical efficiency for spinal blocks. The rapid surge in high volume joint replacement surgeries demands unparalleled efficiency and absolute precision in the operating room. Modern surgical departments face immense pressure to optimize every single minute of their schedules while maintaining the highest standard of clinical excellence. Amidst these intense demands seamless spinal block administration has become more critical than ever before.
Traditionally positioning patients for spinal anesthesia required nurses to act as manual human props. This outdated practice places extraordinary physical strain on the dedicated nursing staff. Extensive OHSU Biodynamics lab testing confirms the extreme dangers of this manual patient handling. The research clearly shows that manual lifting forces nurses into awkward postures that actively contribute to severe musculoskeletal injuries.
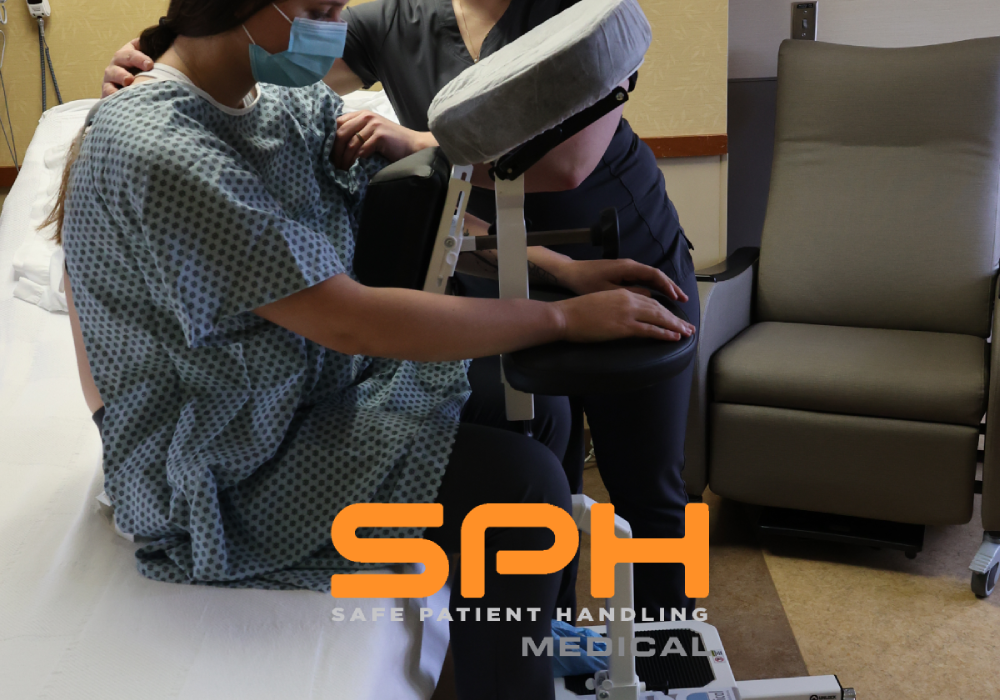
Beyond the severe danger to the healthcare workforce manual positioning creates highly unstable environments for anesthesiologists. A moving target severely compromises the success of the procedure. The Epidural Positioning Device from SPH Medical is the ultimate engineered solution to this critical problem. The EPD provides complete mechanical stability drastically improving procedural efficiency and ensuring the highest level of safety for both patients and surgical staff.
Meeting the Demands of High Volume Joint Replacements
The increasing number of orthopedic procedures such as total knee and hip replacements rely heavily on spinal blocks for optimal patient outcomes. Spinal anesthesia allows for faster recovery times and reduces the systemic impacts associated with general anesthesia. However the success of a busy orthopedic schedule hinges on the rapid and safe administration of these blocks.
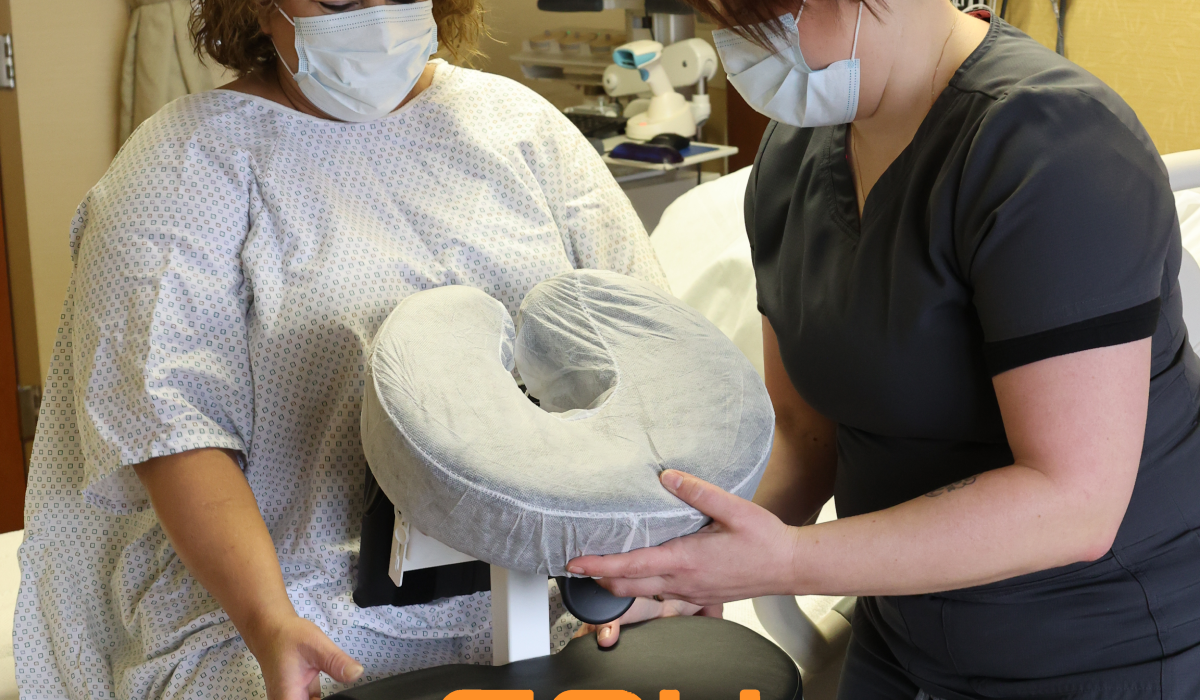
The Epidural Positioning Device accelerates operating room workflow by providing an incredibly intuitive user friendly design. It allows for rapid standardized patient setup before the surgery begins. This technology completely eliminates the massive amount of time wasted scavenging for pillows blankets or makeshift supports. Nurses can position the patient perfectly in a matter of seconds
Streamlining the anesthesia process prevents costly delays and keeps busy operating room schedules running perfectly on time. Every minute saved during the preoperative phase translates to massive financial savings for the hospital. Faster more efficient positioning directly aligns with hospital performance and process improvement goals. By equipping your staff with the best tools available you maximize surgical department efficiency across the board.
Unmatched Stability and Ergonomic Design
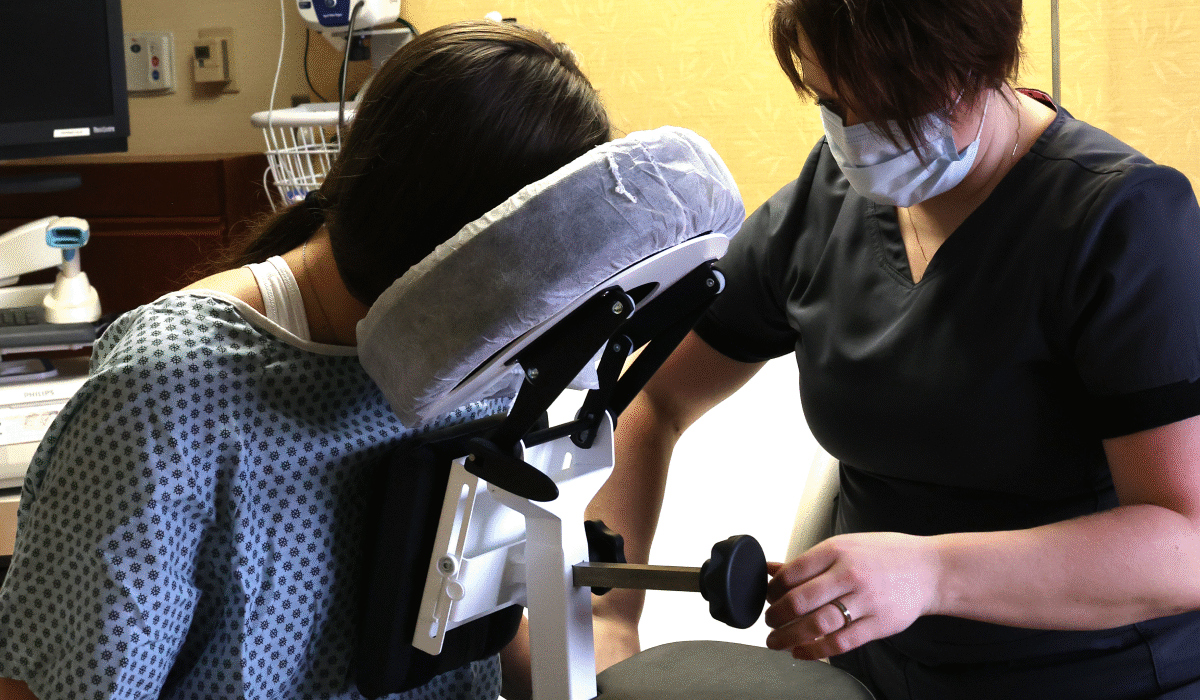
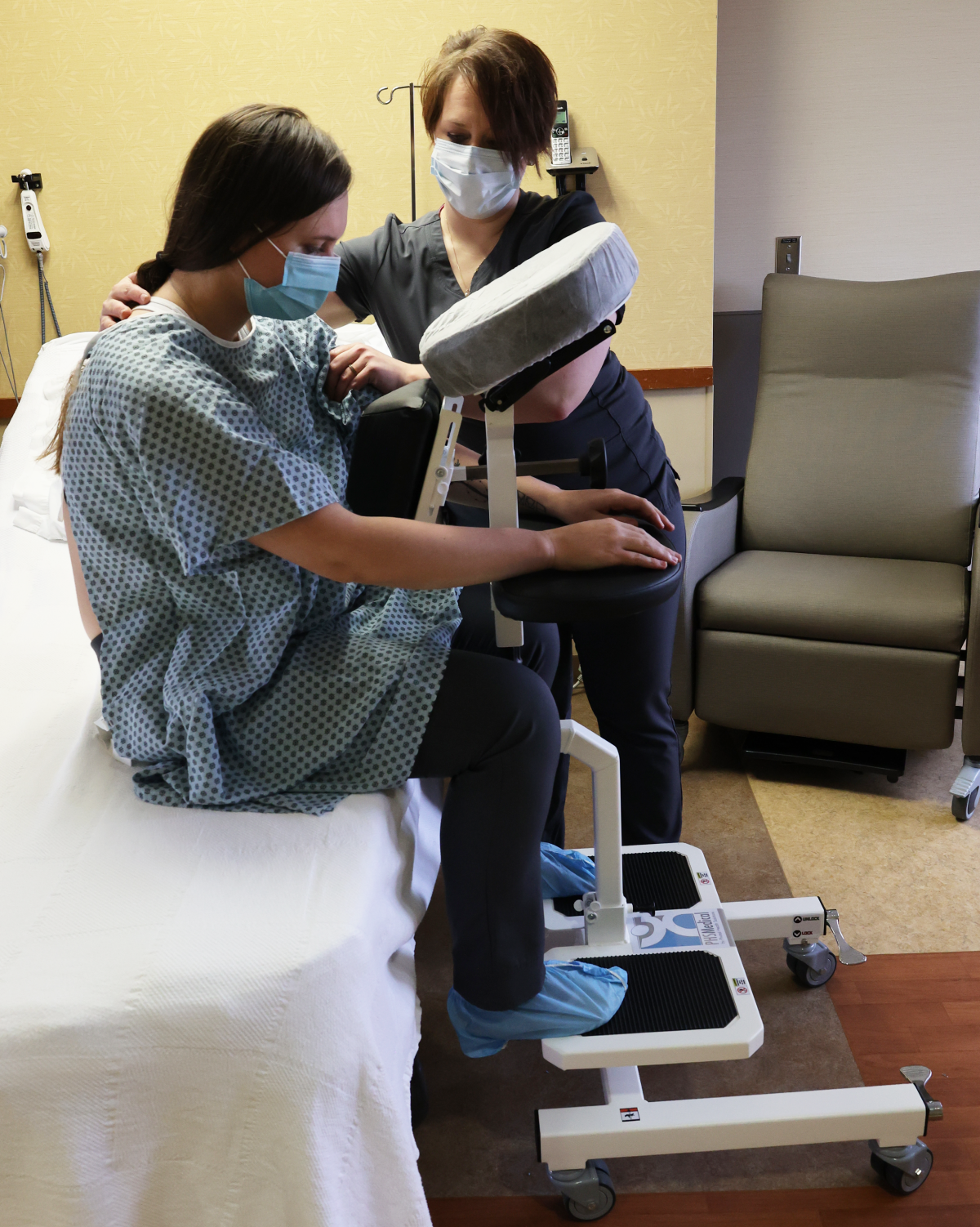
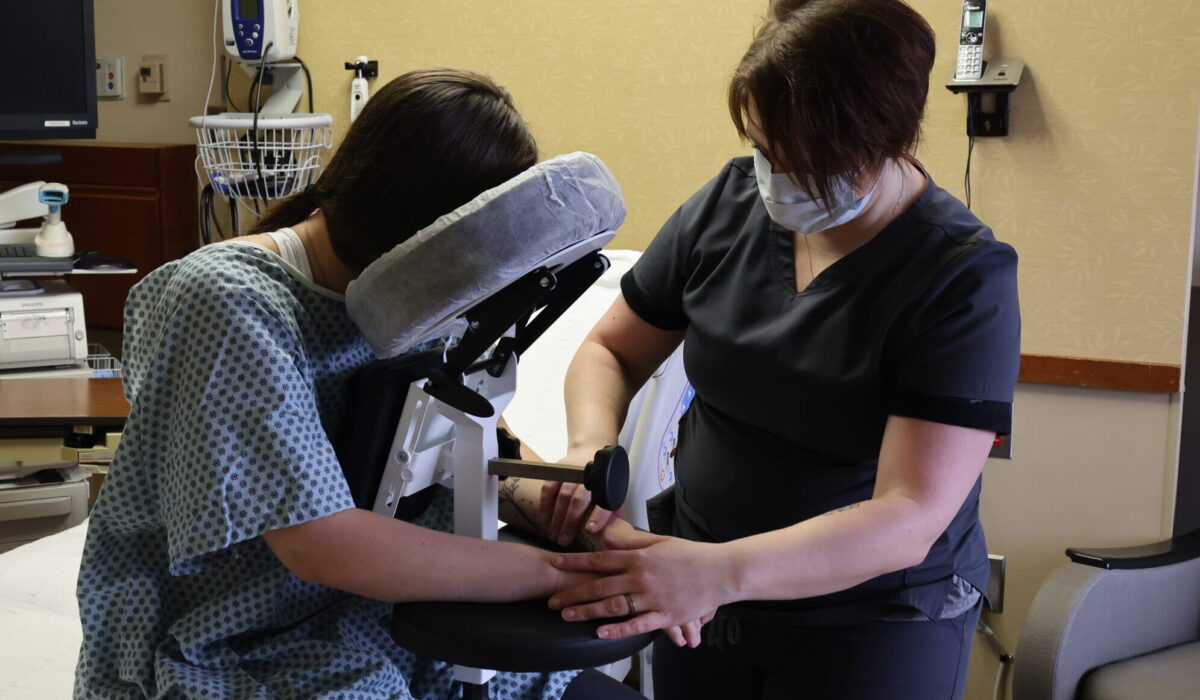
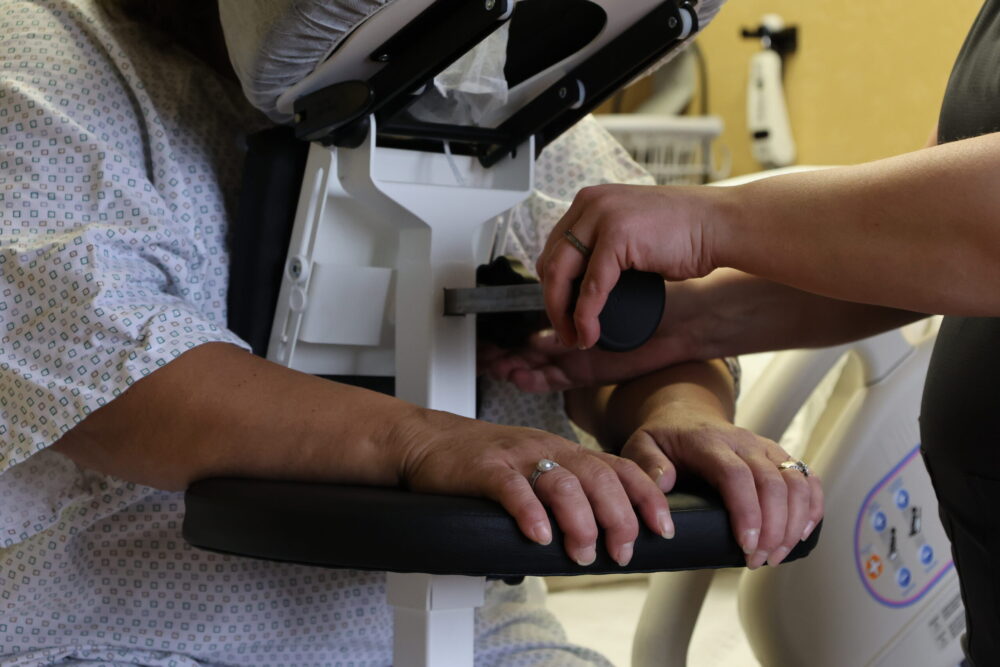
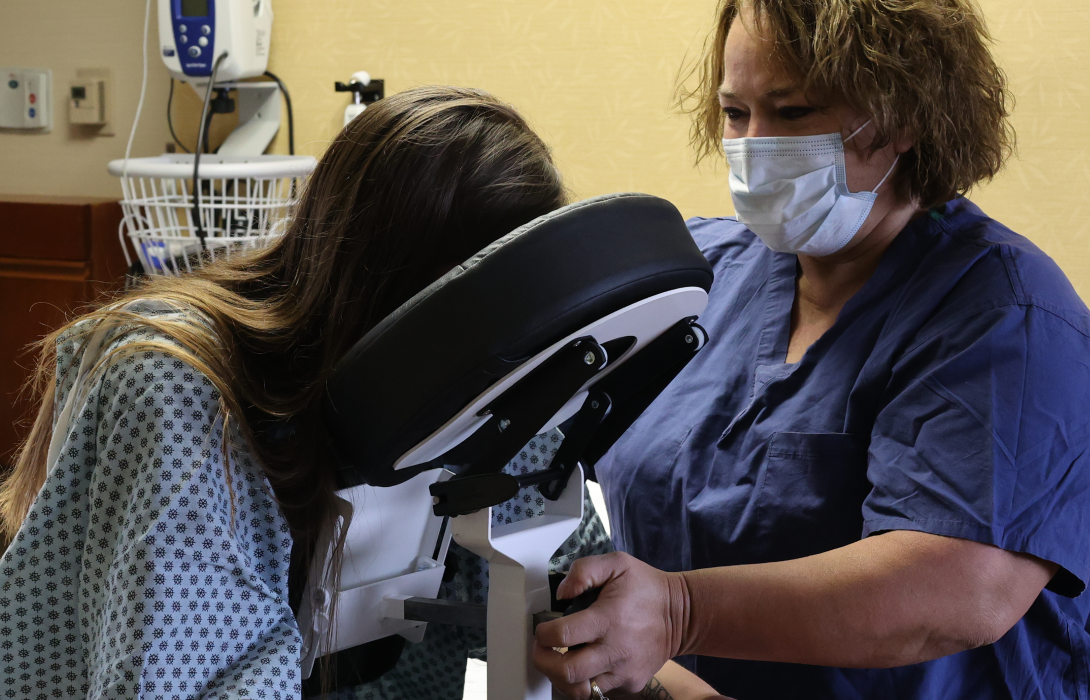
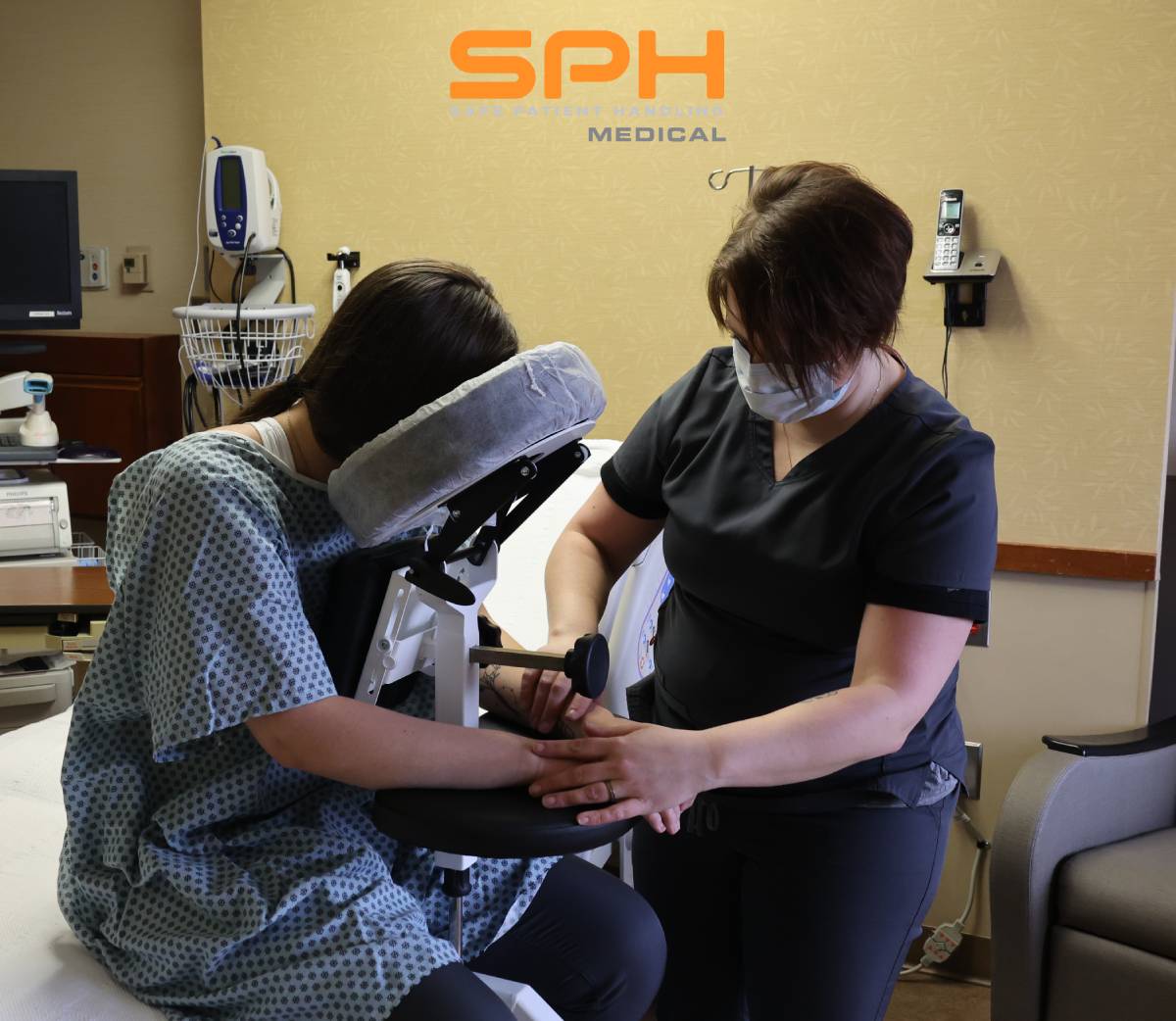
Anesthesiologists require a perfectly still target to safely administer a spinal block. The Epidural Positioning Device provides a rock solid mechanically sound platform that prevents unintended patient movement during needle insertion. When patients feel securely supported they can relax their muscles which naturally opens the intervertebral spaces.
This absolute precision leads to significantly higher first attempt success rates for the anesthesiologist. Achieving the block on the very first try prevents traumatic taps and drastically reduces procedural complications. The rigid stability of the EPD empowers physicians to perform their duties with absolute confidence and unparalleled accuracy.
The device also offers comprehensive ergonomic support through fully adjustable chest arm and head supports. These highly engineered components easily conform to any patient anatomy. The heavy duty construction safely accommodates the rapidly growing bariatric patient population. This ensures equitable high quality care for every individual while removing the physical burden from the nursing staff entirely.
Elevating Patient and Staff Safety
Protecting the nursing workforce must be the top priority for any healthcare facility. Staff injuries are on the rise and require immediate intervention. The Epidural Positioning Device completely eliminates the need for nurses to manually hold patients in awkward static postures. Our solutions enable healthcare professionals to safely lift transfer position and mobilize patients safely while avoiding risk of injury.
Utilizing engineered mobility solutions strictly aligns with ANA APTA and AORN Safe Patient Handling and Mobility safety standards. Years of evidence confirms that Safe Patient Handling programs improve patient and staff safety immensely. This comprehensive support reduces workers compensation costs and minimizes lost work days by preventing severe back and shoulder injuries among clinical staff.
Furthermore the Epidural Positioning Device greatly enhances patient comfort and clinical outcomes. A secure mechanically supported resting position reduces patient anxiety and eliminates the profound fear of falling. Comfortable stable positioning minimizes ischemic pain and drastically improves overall patient satisfaction scores. Elevating the patient experience is a key success indicator for every modern hospital.
Comprehensive Training and Seamless Integration
SPH Medical understands that introducing new technology requires comprehensive support. We offer extensive inservice videos and skill check lists to help keep your skills and knowledge completely up to date. Our dedicated team ensures that all staff members are fully equipped to utilize the Epidural Positioning Device effectively from day one.
The user friendly adjustability and intuitive features ensure that the device integrates seamlessly into your existing operating room workflows. There is no steep learning curve or complicated setup process. The EPD is designed specifically for the fast paced demands of a high volume surgical department.
By standardizing the positioning process hospitals can ensure consistent predictable outcomes for every single procedure. This level of reliability is absolutely essential for maintaining clinical excellence and achieving your critical performance metrics.
The Ultimate Standard of Care with the EPD for Spinal Blocks
The Epidural Positioning Device represents a massive leap forward in operating room technology. It serves as a powerful catalyst for reducing procedural delays and accelerating the surgical schedule. Investing in this advanced equipment demonstrates an uncompromising commitment to clinical safety and operational superiority.
Hospitals that implement the EPD see immediate measurable improvements in both staff morale and procedural efficiency. Nurses no longer face the physical dread of manually supporting heavy sedated patients. Anesthesiologists praise the rigid stability that allows them to perform their blocks flawlessly.
This device is the definitive standard of care for modern surgery departments. It transforms the administration of spinal blocks by delivering unmatched stability superior ergonomic design and comprehensive safety for clinical staff. Do not allow outdated dangerous manual handling practices to compromise your surgical outcomes or threaten your valuable nursing workforce.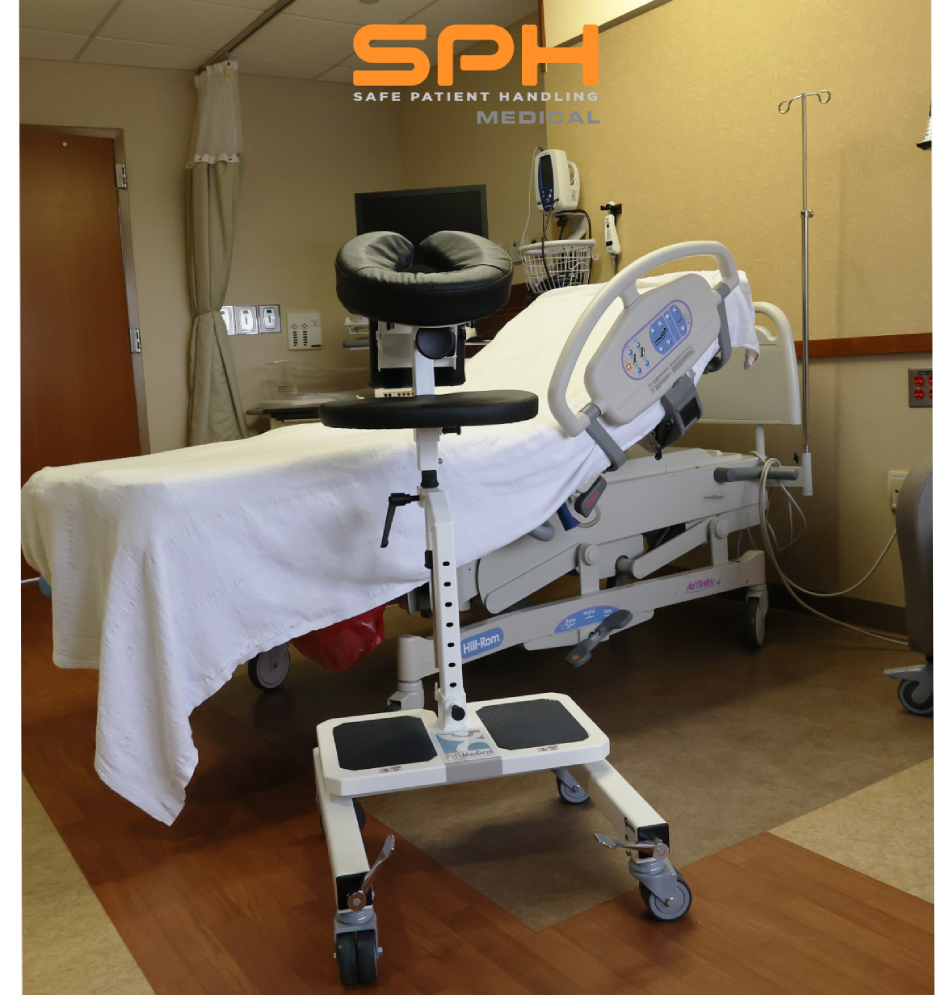
Transform Your Surgery Department Today
Your surgical staff deserves the highest level of mechanical support available. The Epidural Positioning Device is the exact tool required to meet the escalating demands of high volume joint replacement surgeries. It protects your nurses empowers your physicians and ensures maximum comfort for your patients.
Do not compromise on operating room efficiency or staff safety for another single day. Elevate your standard of care and experience the unmatched benefits of true mechanical stability.
Contact SPH Medical today to request a quote for the Epidural Positioning Device. Our team is ready to help you implement this revolutionary technology and immediately elevate the standard of care in your surgical department.