No Room for Error When It Comes To Staff Safety
It’s hard to imagine health care without anesthesia or analgesia. Even after 175 years, they’re a medical marvel that no one takes for granted. Technology and innovation may evolve at lightning speed, but there are still no shortcuts during epidurals and spinal blocks. Whenever anesthetists place a needle in a patient, they summon all their knowledge, training, skill, experience and powers of concentration. Where the spinal cord and nerve roots are concerned, there’s no room for error. Simply put, if epidural placement is inaccurate, pain is the least of anyone’s worries.
Positioning the Patient: What’s the Problem?
There’s more to getting pain medicine to the right place than most people realize. Before the needle can be positioned, the patient must be positioned. That’s almost always easier said than done, especially when the patient is elderly or feeble, has difficulty following instructions, or outweighs the assisting nurse. That last scenario is quite common and highly problematic.
In 2016, according to the U.S. Bureau of Labor Statistics, nurses were injured on the job at a significantly higher rate than full-time workers in other occupations. Fifty-one percent of injuries involved muscle strains, sprains or tears, and more than a fourth of those were back-related. The average recovery time away from work was seven days.
Work-related MSDs, or musculoskeletal disorders, are injuries caused by lifting or overexertion. In 2016, MSDs accounted for a whopping 44 percent of RNs’ occupational injuries.
Needless to say, if nurses go down, the whole system goes down. Maybe you’ve never given or received epidurals and spinal blocks. If not, you’re probably thinking, “How hard can it be to tell a patient how to sit?”
Well, it’s a little like telling a ballerina to hold a picture-perfect arabesque while the photographer tries different angles.
That’s an extreme example, but the point is this: Patients are asked to assume an unnatural position and sustain it throughout a tricky procedure that can’t be rushed. Incredibly, some rather primitive methods are still employed.
The Perils of Manual Positioning
To achieve the ideal position, it’s not uncommon for staff members to prop up patients on rickety bedside tables and unwieldy pillows. Nurses and anesthesiologists who lack state-of-the-art equipment must be resourceful.
With any luck, the bedside table won’t collapse or tip. Hopefully, the pillows won’t slip to the floor with the patient close behind. Women receiving epidurals before hard labor, even those who avoid injury, are in no mood for such nonsense. The assisting staff member could easily become the next patient.
Given all the things that could go wrong with manual positioning, it’s easy to see why EPD use is becoming more widespread.
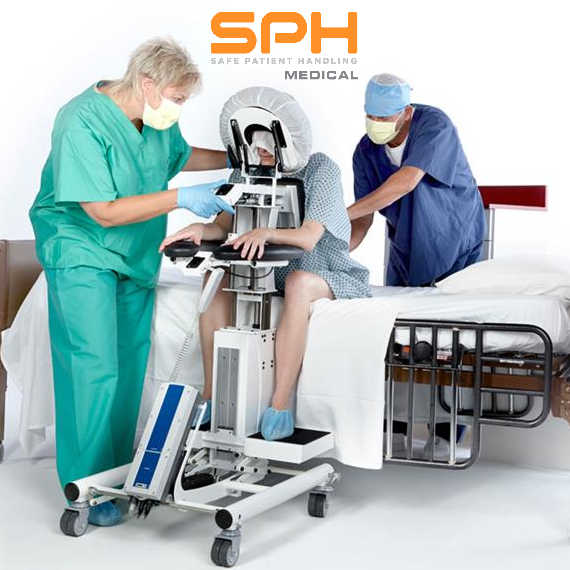
The Epidural Positioning Device
For epidurals and spinal blocks it is necessary, the EPD (epidural positioning device) is a godsend. The design takes several things into account:
- Ease and accuracy of epidural placement.
- Patient stability and comfort.
- Weight support up to 600 pounds.
- Portability.
- Staff safety.
The epidural positioner is not just a luxury item any more than a seat belt is a nice accessory for a car. EPDs make it easier for anesthesiologists to do their job. EPDs keep nurses healthy and on top of their game. EPDs help patients receive first-rate care with optimal outcomes. Given all those benefits and more, EPDs are increasingly considered necessary.
The Epidural Positioner in Thoracentesis
EDPs are widely used in labor and delivery, surgery and orthopedics. They are even useful in radiology departments.
Thoracentesis, also known as pleural tap, is a procedure to remove excess fluid in the lungs. A little fluid is appropriate for lubrication; it keeps the membranes involved in breathing from rubbing together. However, too much fluid interferes with lung capacity. Labored breathing and pain result. Excess fluid can also interfere with imaging or diagnosing disease.
In any case, thoracentesis also requires careful patient positioning and needle placement. During Thoracentesis patients must be supported in a comfortable position over a prolonged period while drainage occurs. Radiologists and their imaging teams are thankful for the EPDs that make their jobs easier and prevent injuries.
The uses and benefits of the epidural positioner become more apparent all the time. This is one innovation that will be around for a while.
https://www.bls.gov/opub/mlr/2018/article/occupational-injuries-and-illnesses-among-registered-nurses.htm