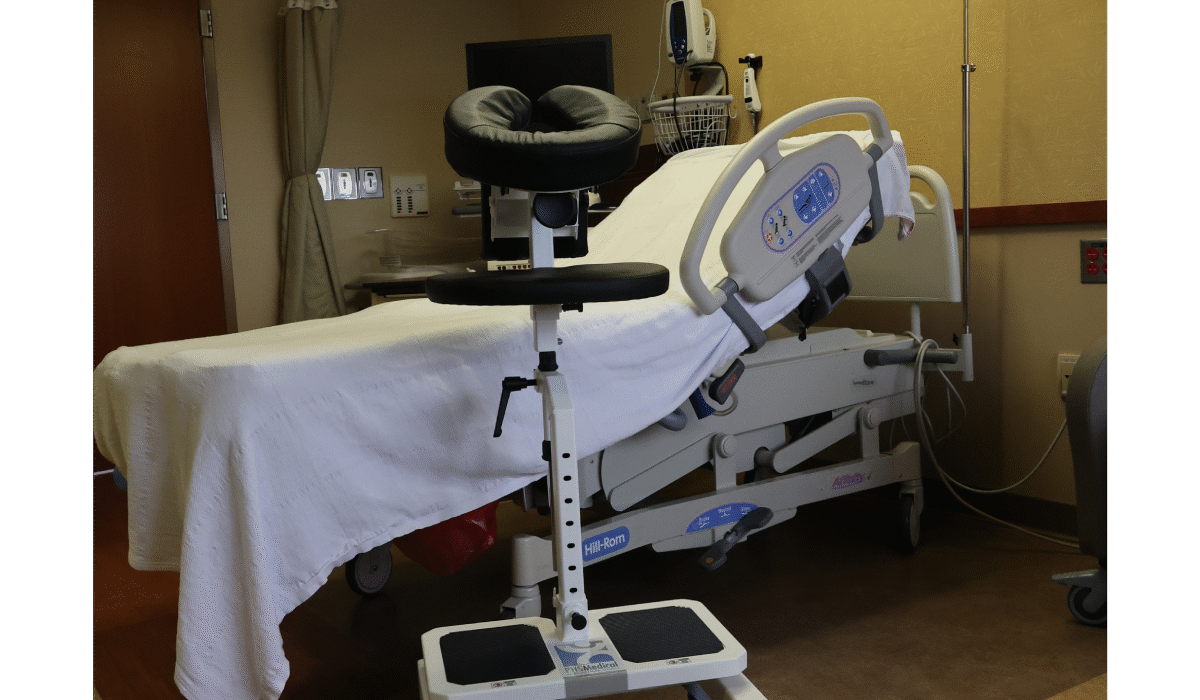
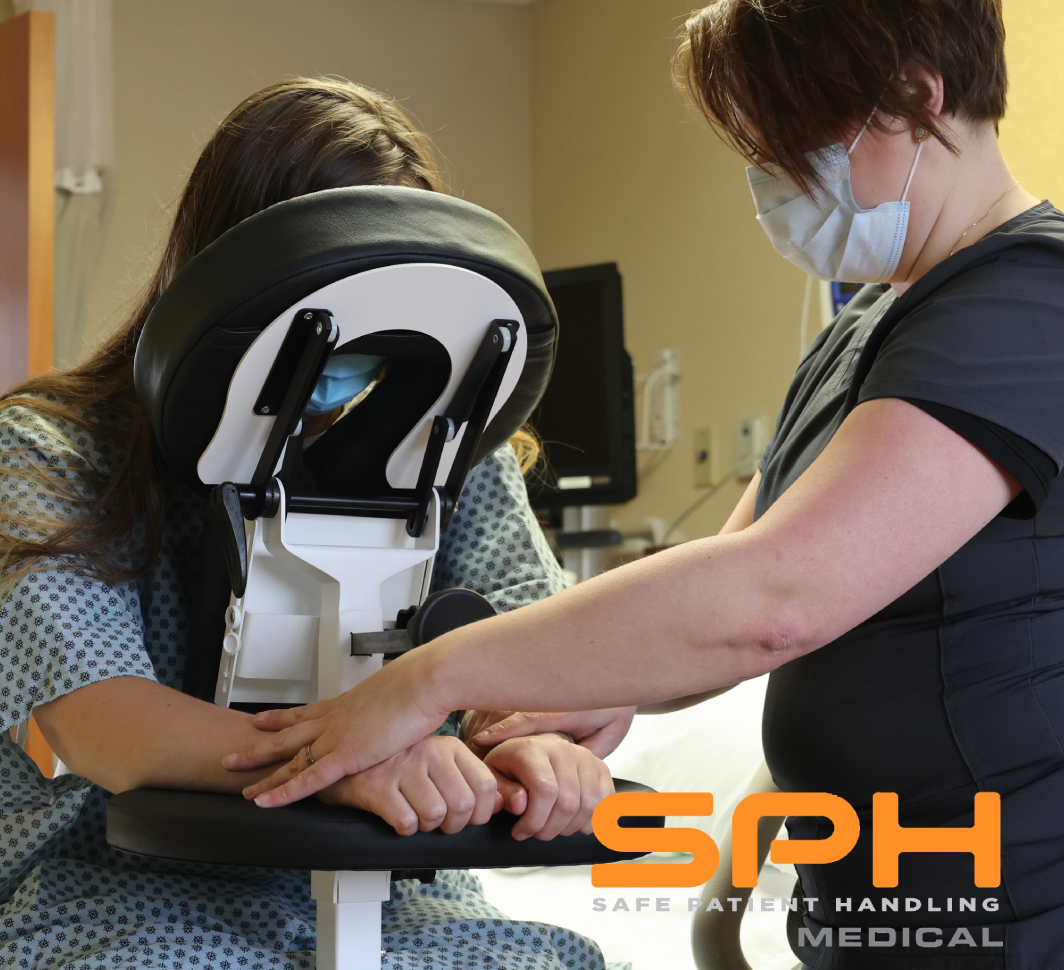
Portable Parallel Bars in Rehabilitation Mobilizing Patients Anywhere
Prolonged immobility in the hospital setting is a devastating clinical liability. When patients remain confined to their beds they rapidly lose muscle mass and face a severe risk of developing secondary complications. Initiating early safe patient mobility is the absolute most effective strategy to reduce hospital length of stay and drive superior patient outcomes. However mobilizing patients is not without significant challenges. Physical therapists and nurses face extreme risks when manually handling high acuity and bariatric patients.
Extensive OHSU Biodynamics lab testing confirms the severe danger of manual patient handling versus the use of highly engineered assistive devices. Relying on outdated manual techniques actively contributes to catastrophic musculoskeletal injuries among healthcare workers. The definitive solution to this escalating crisis is providing your staff with the absolute best mechanical support available.
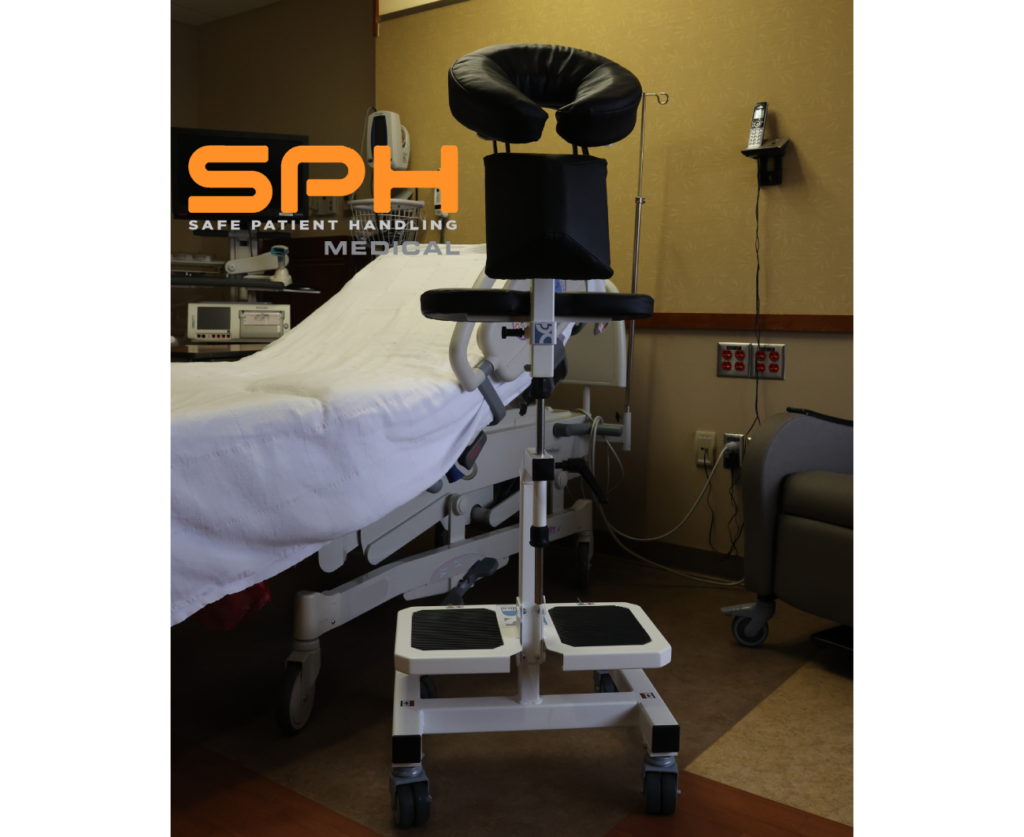
SPH Medical Portable Parallel Bars represent the highest standard in flexible rehabilitation equipment. This innovative technology enables healthcare professionals to safely lift transfer position and mobilize patients absolutely anywhere while entirely avoiding the risk of injury. By integrating this equipment into your facility you enhance patient safety protect your workforce and achieve your most critical process improvement goals.
The Critical Imperative for Early Mobility Programs
Implementing a comprehensive early mobility program is a fundamental requirement for modern healthcare facilities. The benefits of getting patients upright and moving as soon as clinically possible are supported by decades of irrefutable evidence.
Accelerating the Healing Process with SPH Medical Portable Parallel Bars
Early weight bearing exercises are essential for preventing severe muscle atrophy. When patients are mobilized early they maintain their functional strength which accelerates the entire healing process. Furthermore upright positioning and movement serve as highly effective interventions for pressure ulcer prevention. Immobility is a primary driver of skin breakdown and early mobility perfectly complements the stringent standards of wound care nurses.
Accelerating the healing process has a direct massive impact on hospital operations. Shorter hospital stays directly reduce overall hospital costs and free up critical bed space for new admissions. Aligning your rehabilitation practices with early mobility protocols ensures that your facility achieves its performance and process improvement goals rapidly and consistently.
Aligning with National Safety Standards
Protecting your staff is just as important as protecting your patients. Utilizing engineered mobility solutions strictly aligns with ANA APTA and AORN Safe Patient Handling and Mobility safety standards. Years of evidence confirms that Safe Patient Handling programs improve patient and staff safety immensely.
When facilities provide comprehensive support tools like Portable Parallel Bars they see an immediate reduction in staff injury rates and severity. This directly leads to massive workers compensation cost reduction. Lost work days for staff are reduced drastically preserving your highly skilled workforce and boosting overall department morale.
Unmatched Features of SPH Medical Portable Parallel Bars
To truly mobilize patients anywhere the equipment must be exceptionally engineered. SPH Medical Portable Parallel Bars deliver unparalleled performance through a combination of supreme stability exceptional portability and precision adjustability.

Supreme Stability and Safety
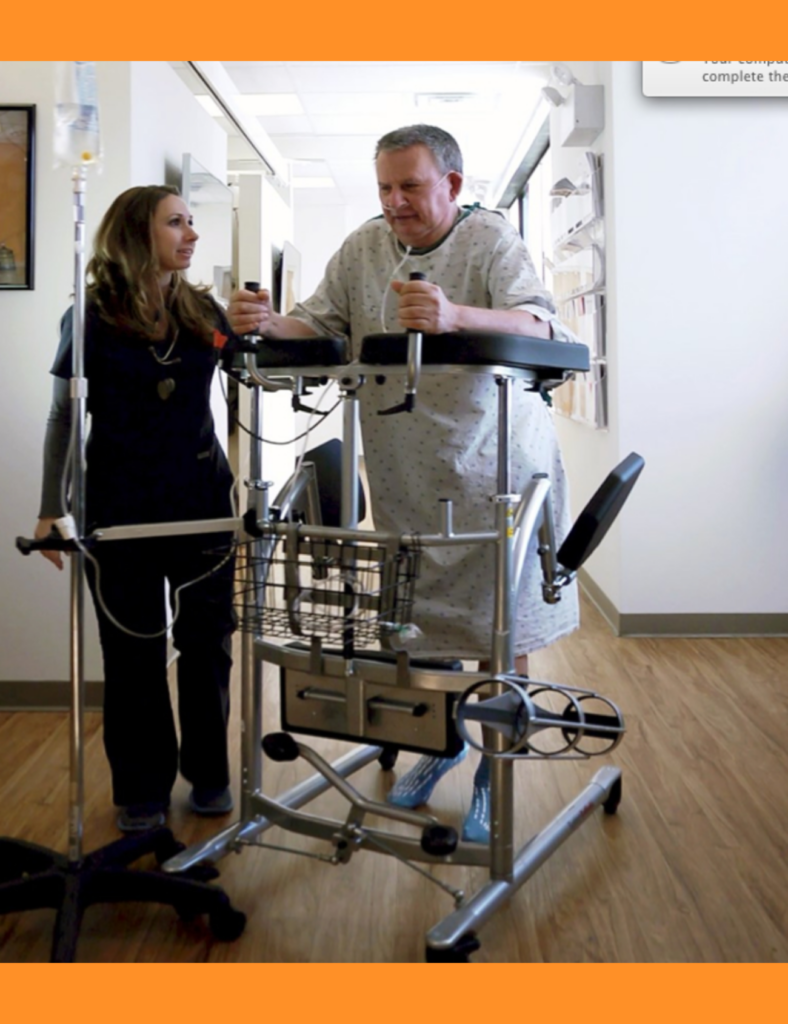
The foundation of effective gait training is absolute stability. Our Portable Parallel Bars feature a robust heavy duty construction that provides a rock solid foundation for patients taking their first critical steps. This rigid stability entirely eliminates the profound fear of falling that holds many patients back from participating fully in their therapy sessions.
Furthermore this absolute stability completely removes the dangerous need for physical therapists to act as manual human props. When the equipment provides the support the therapist can focus entirely on gait mechanics and functional improvement rather than expending all their energy trying to keep a heavy patient upright. This drastically reduces staff injury rates and ensures a completely secure environment for the rehabilitation session.
Exceptional Portability for Seamless Integration
The most innovative feature of these parallel bars is their exceptional portability. Traditional parallel bars are bolted to the floor in the physical therapy gym. This forces highly vulnerable high acuity patients to be transported long distances just to receive foundational gait training.
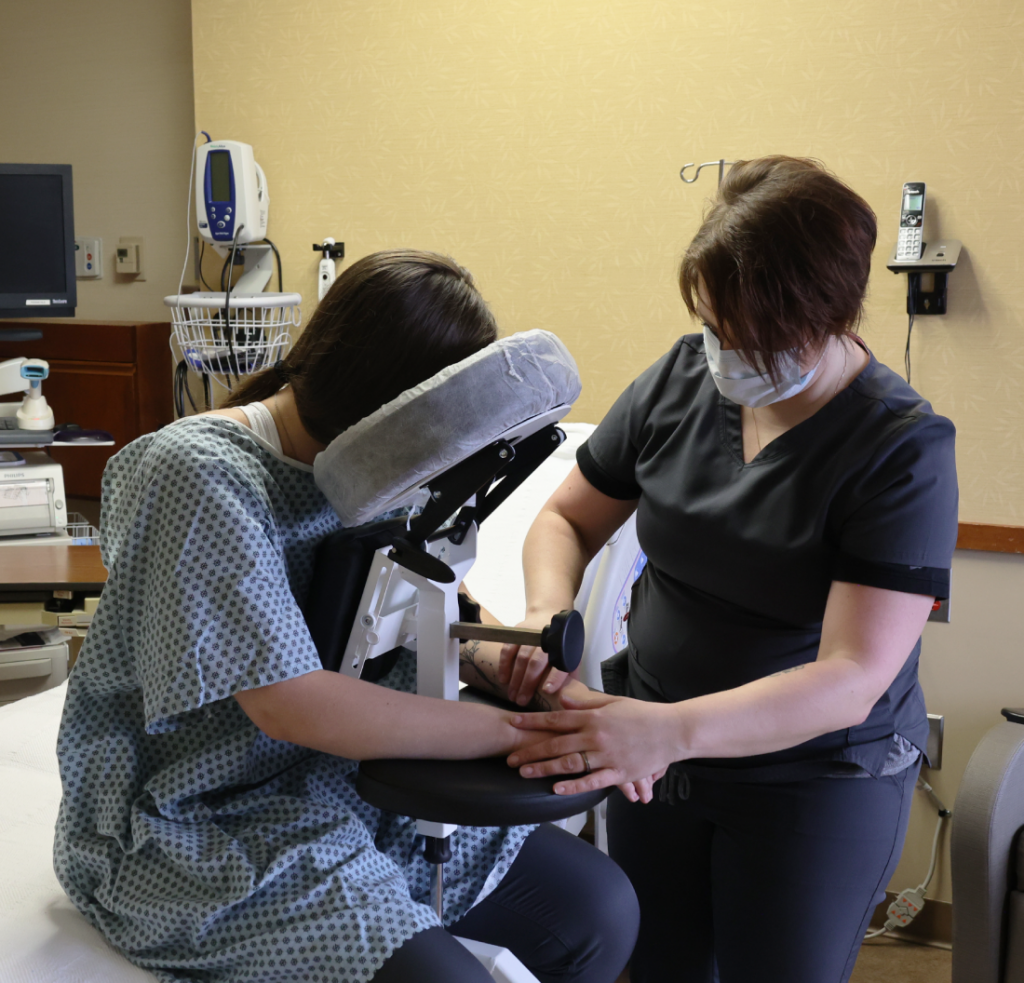
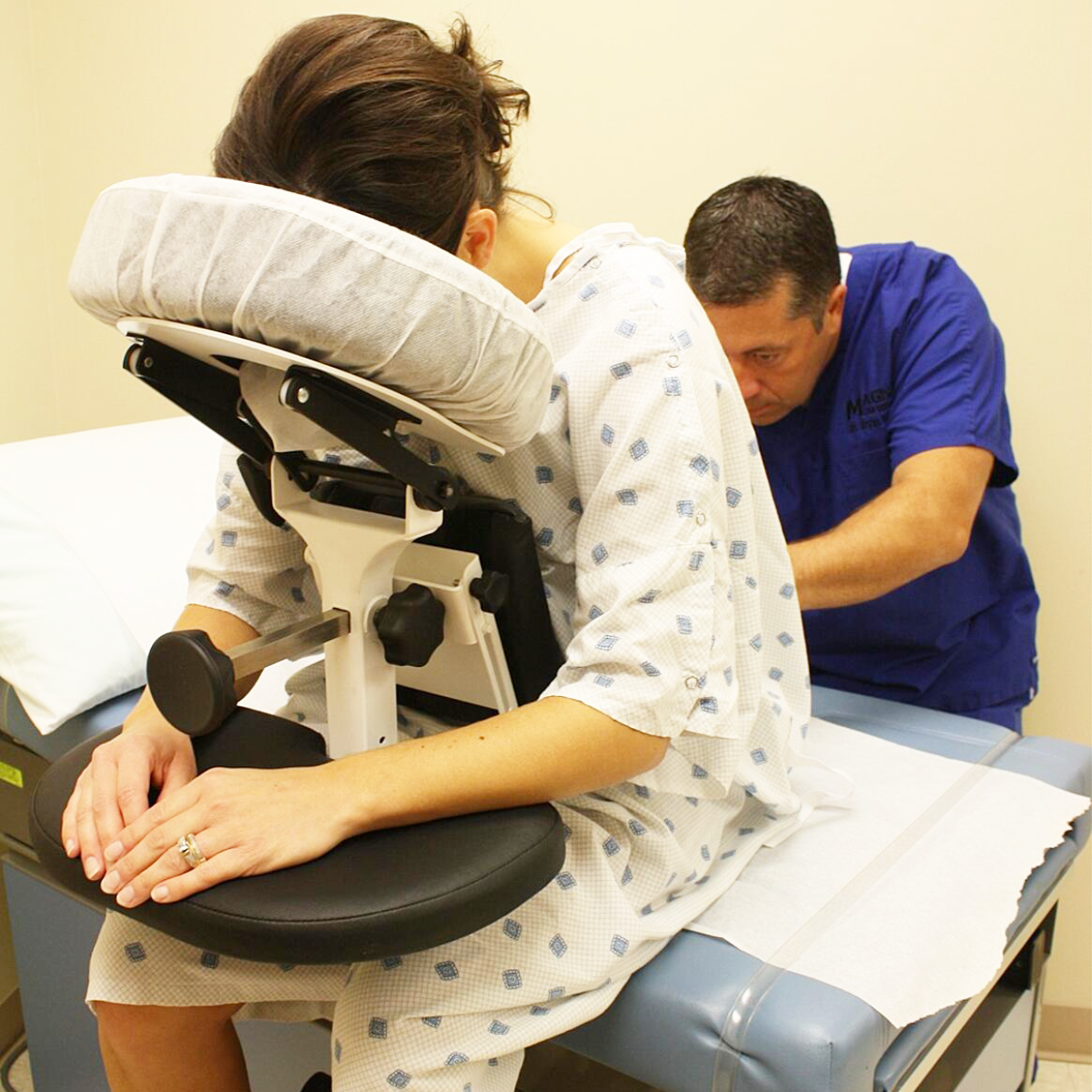
Our Portable Parallel Bars feature an incredibly innovative design that allows the equipment to be easily transported and set up in any patient room intensive care unit or dedicated physical therapy department. This seamless integration ensures that patients who cannot travel to the gym still receive essential early gait training. You can bring the absolute highest standard of rehabilitation directly to the bedside.
Precision Adjustability
Every patient has unique anatomical needs and our equipment adapts to them flawlessly. The Portable Parallel Bars feature an intuitive user friendly interface that allows for rapid height and width adjustments. Therapists can customize the exact ergonomic support required for each individual in a matter of seconds.
This precision adjustability includes the ability to safely accommodate the growing bariatric patient population. Providing equitable high quality care for patients of all sizes is a critical mandate for modern hospitals. Our heavy duty adjustable bars ensure that every patient receives the exact support they need to succeed in their recovery journey.
Elevating Patient Outcomes and Staff Confidence
Investing in the highest standard of rehabilitation equipment delivers profound measurable returns across your entire organization. It transforms the patient experience and empowers your clinical staff to perform at their absolute best.
Portable Parallel Bars; Empowering the Patient
A secure mechanically supported environment builds immense patient confidence during foundational gait mechanics training. When patients feel safe and protected they are far more willing to push themselves during therapy. This increased confidence leads directly to higher patient compliance with rehabilitation protocols.
Higher compliance translates to faster recovery timelines and earlier discharge dates. Moreover providing a comfortable secure rehabilitation experience drastically improves overall patient satisfaction scores. Patients recognize and appreciate when a facility invests in their safety and comfort.
Protecting the Healthcare Workforce
Your clinical staff is your most valuable asset. Replacing dangerous manual lifting with advanced assistive devices is the absolute only way to protect them from career ending injuries. Relying on outdated equipment and manual handling is a severe liability that modern facilities simply cannot afford.
Providing the absolute best equipment boosts staff morale significantly. Nurses and physical therapists feel valued and protected when they have access to state of the art tools. This leads to comprehensive adherence to safety protocols and a culture of continuous process improvement throughout your entire organization.
Portable Parallel Bars are not merely an optional upgrade for your physical therapy department. They are a fundamental absolute requirement for comprehensive early mobility and safe patient handling programs. Decades of clinical evidence confirms that utilizing highly engineered assistive devices is the only way to improve patient and staff safety simultaneously.
The non negotiable standard of care demands that hospitals stop relying on outdated equipment that compromises safety and extends patient recovery times. SPH Medical provides the innovative solutions required to meet the complex demands of modern healthcare.
Do not allow dangerous manual handling practices to threaten your dedicated staff or delay your patients from returning home. Enhance patient safety and elevate your rehabilitation capabilities today. Contact SPH Medical to request a quote for Portable Parallel Bars and integrate seamlessly into your facility early mobility program.