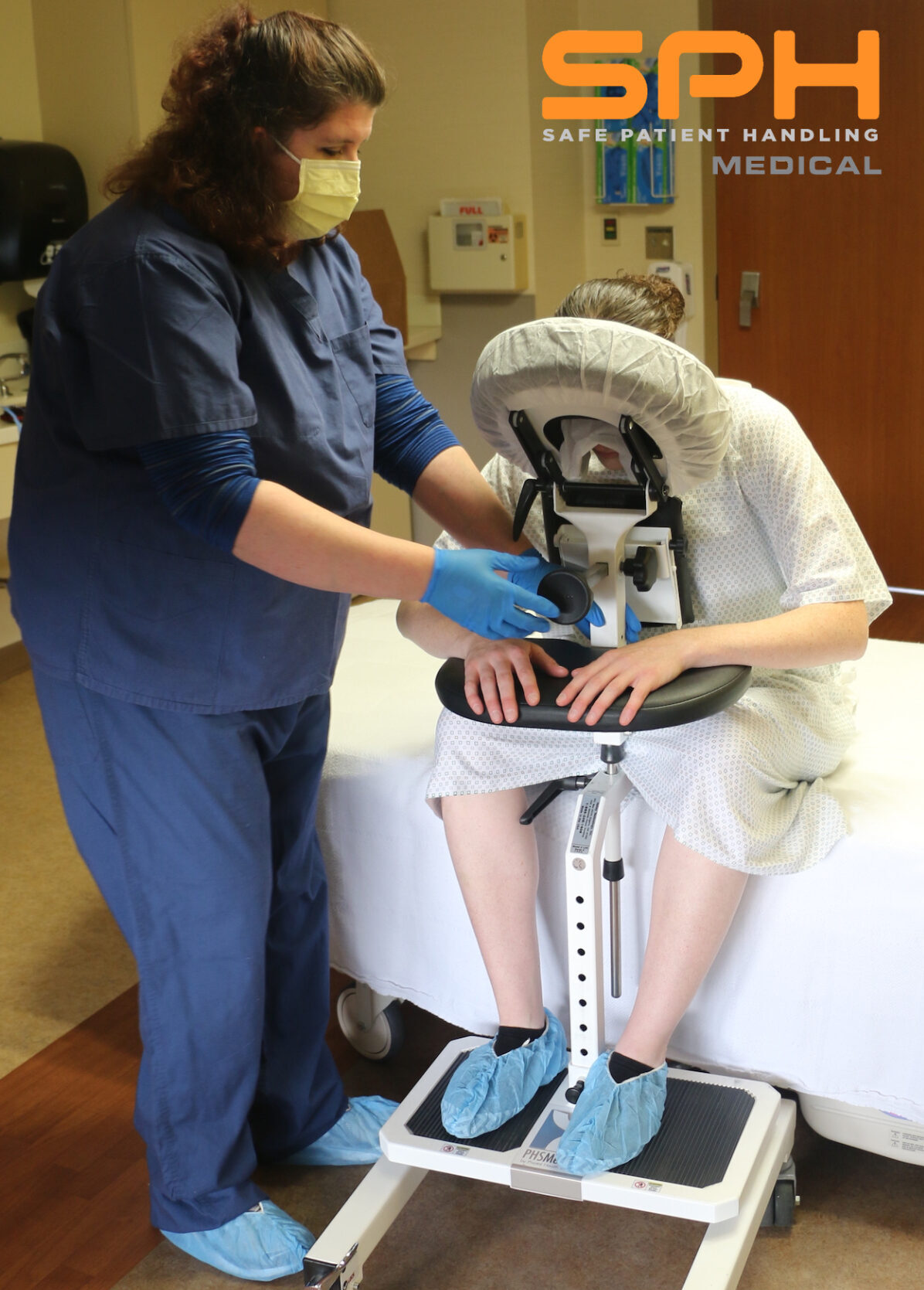
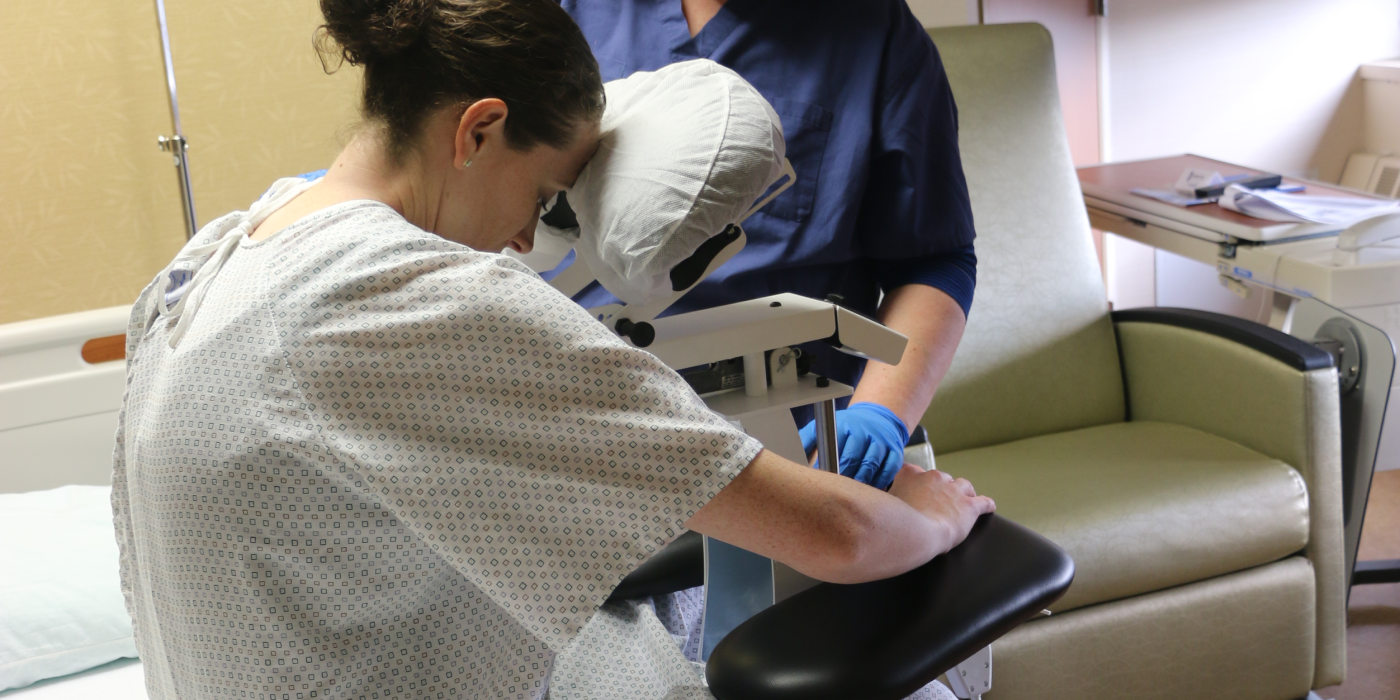
The Definitive Standard for Patient Positioning: Maximizing Safety and Precision with the Epidural Chair
Precise patient positioning is the absolute cornerstone of successful interventional procedures. Whether an anesthesiologist is placing an epidural in a bustling delivery ward or a radiologist is performing a delicate spinal block, the margin for error is nonexistent. For decades, healthcare professionals have relied on outdated, unsafe methods to achieve this positioning. Nurses and physical therapists are routinely forced to act as “human props,” manually holding patients upright and still.
This outdated approach puts everyone at risk. Manual patient handling leads to severe musculoskeletal injuries for staff, while unstable positioning compromises procedural accuracy for physicians. Biomechanical testing consistently confirms the extreme dangers of manual patient handling compared to the use of highly engineered assistive devices.
The ultimate solution to this critical challenge is the Epidural Chair. This highly advanced, uniquely engineered device represents the most innovative and comprehensive approach to patient positioning. It is designed to enhance patient safety, completely protect healthcare staff from injury, and guarantee unmatched procedural precision across multiple hospital departments.
Engineered for Excellence: Core Features of the Epidural Chair
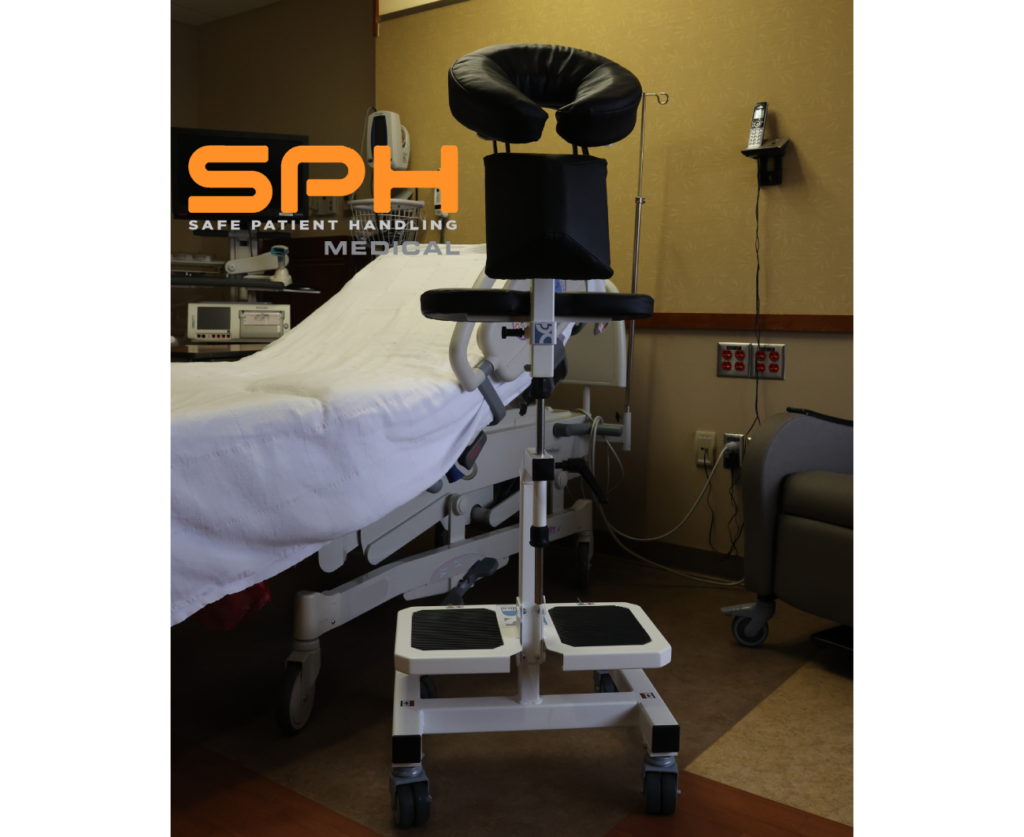
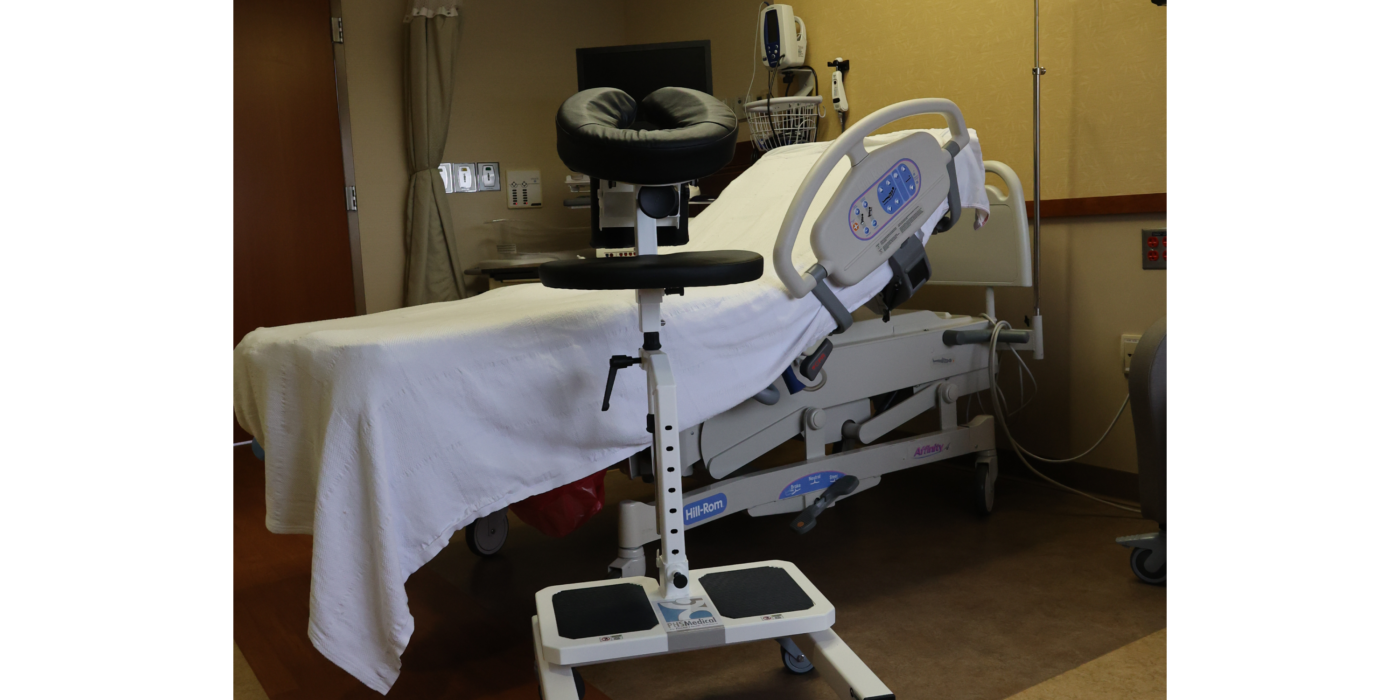
The Epidural Chair replaces the dangerous instability of bedside tables and stacked pillows with a rock-solid, mechanically sound platform. It provides the highest level of support for patients while completely removing the physical burden from your nursing staff.
Unmatched Ergonomic Support
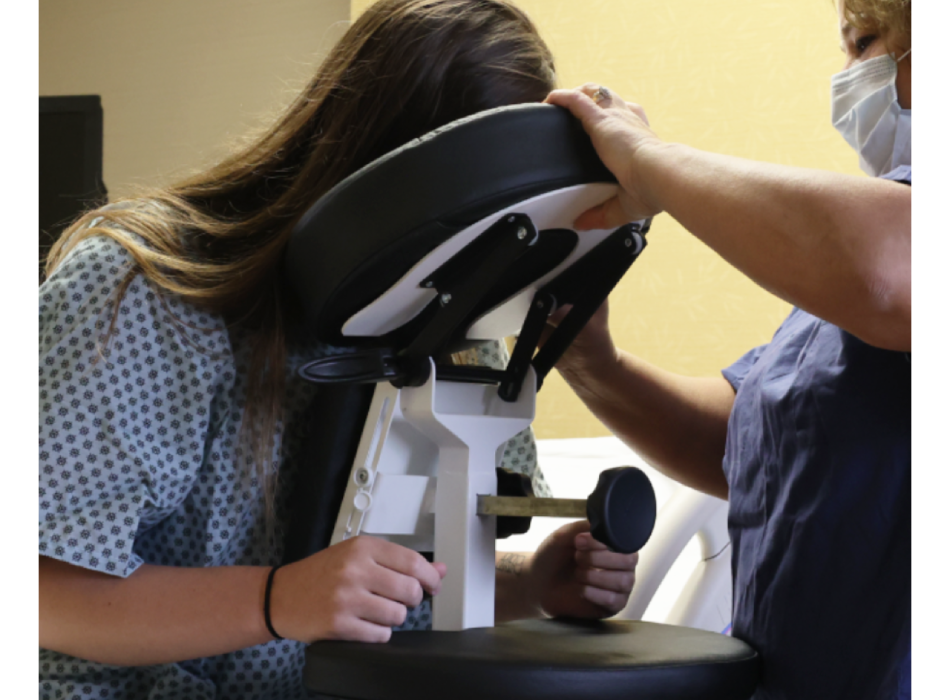
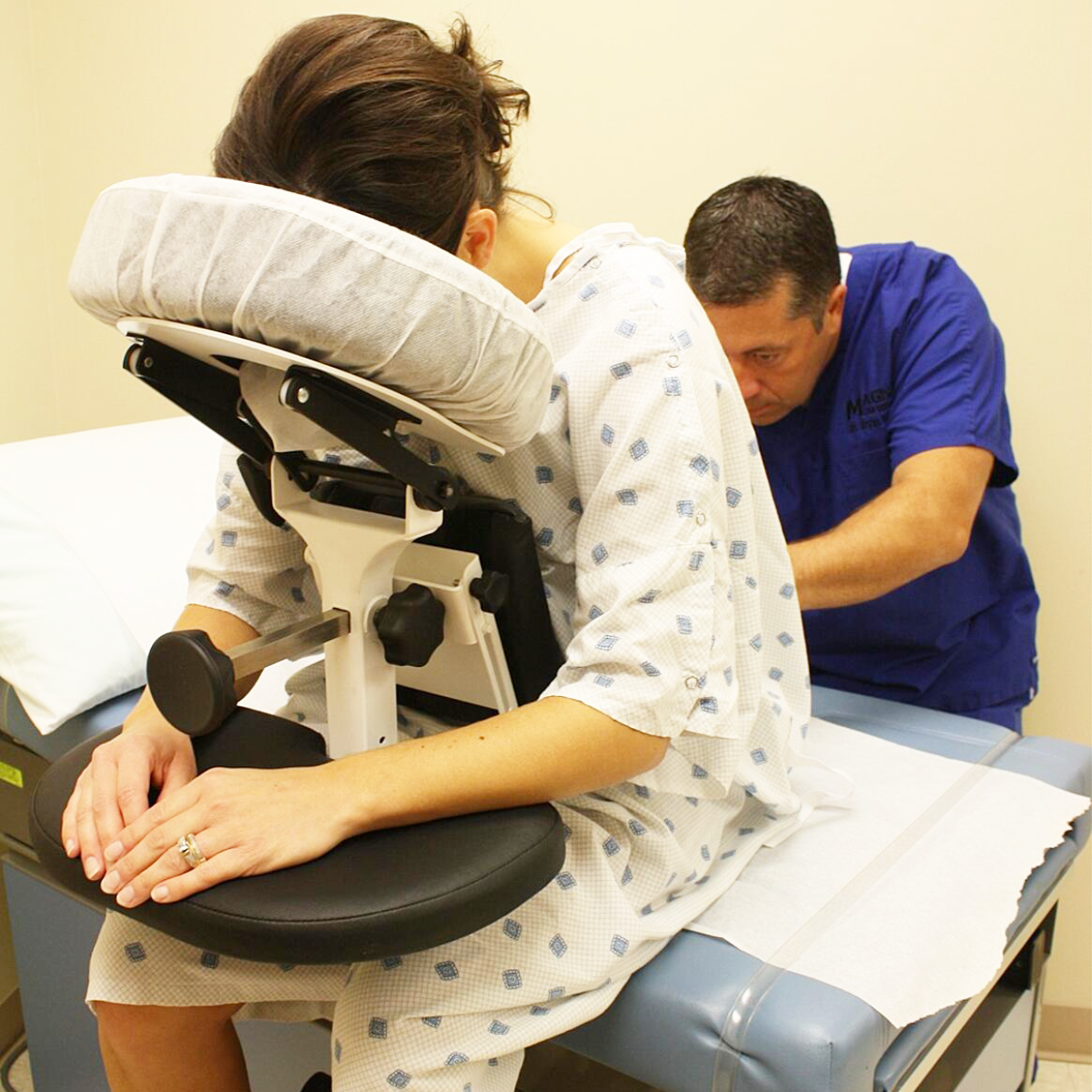
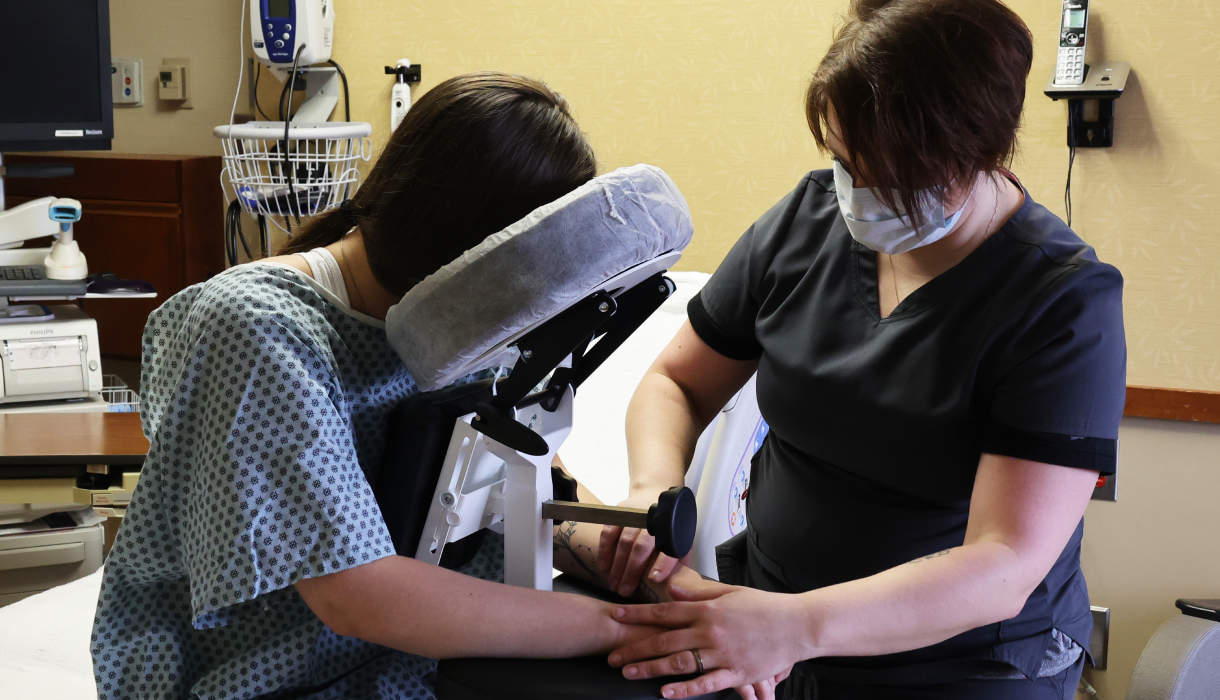
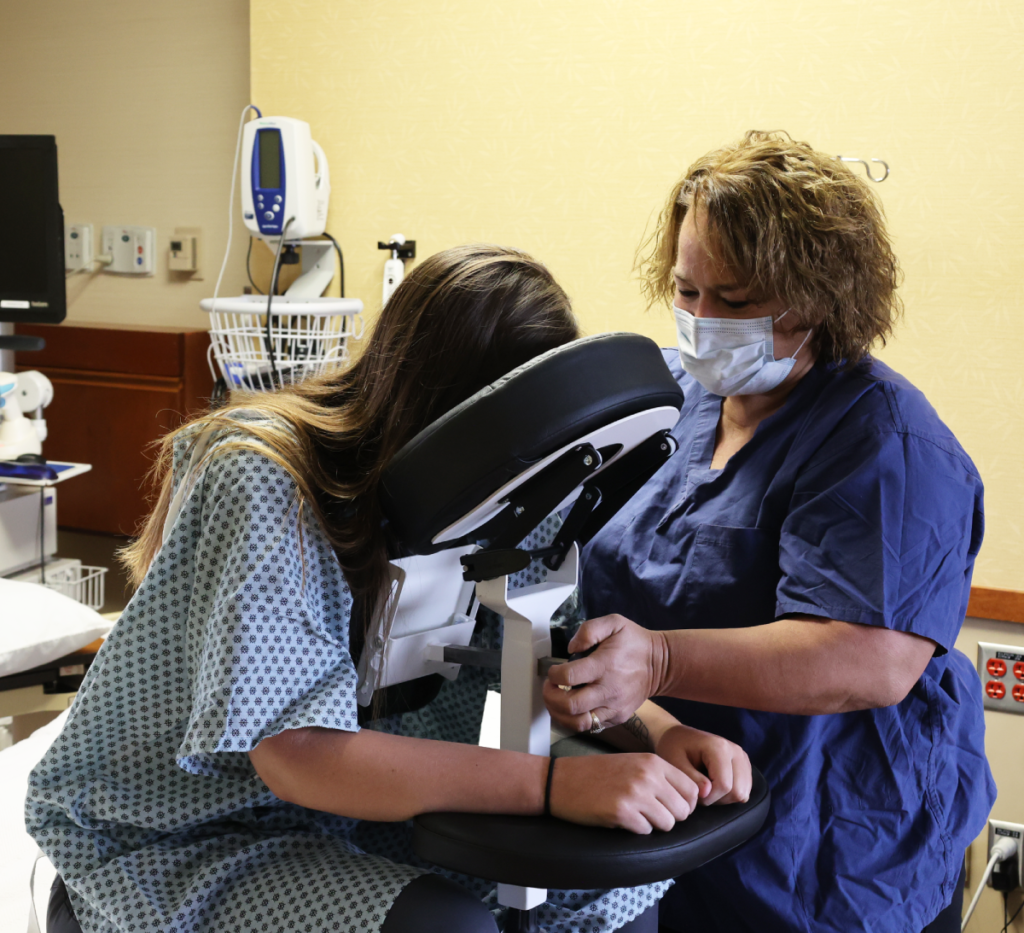
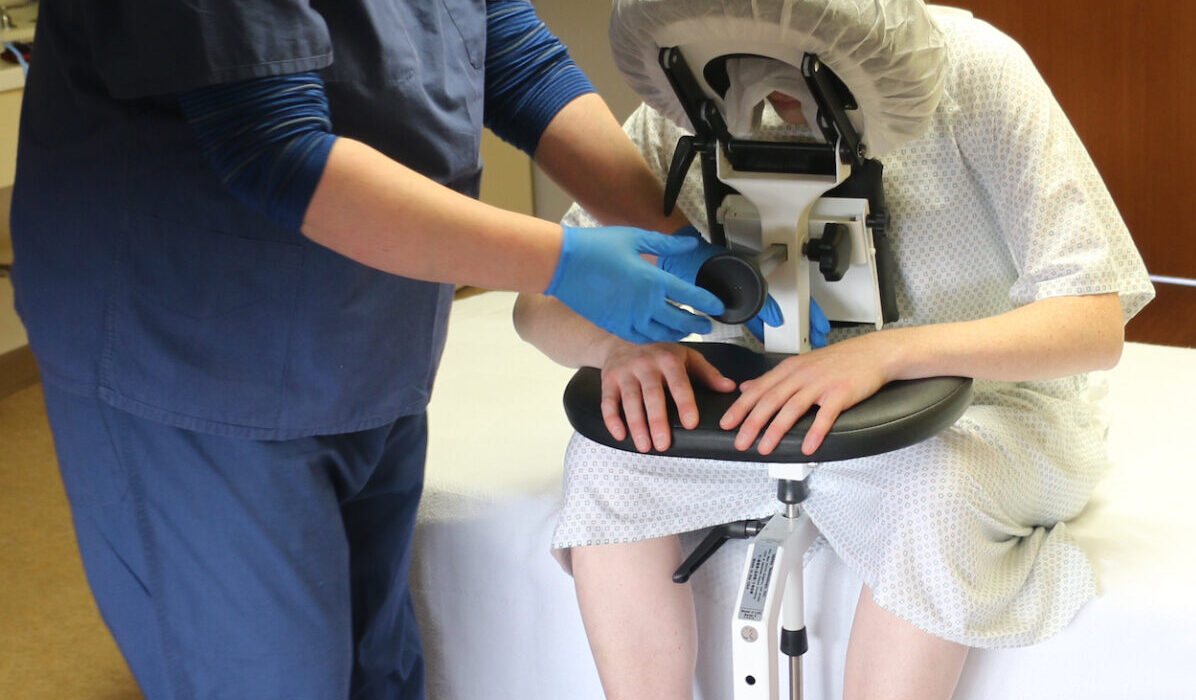
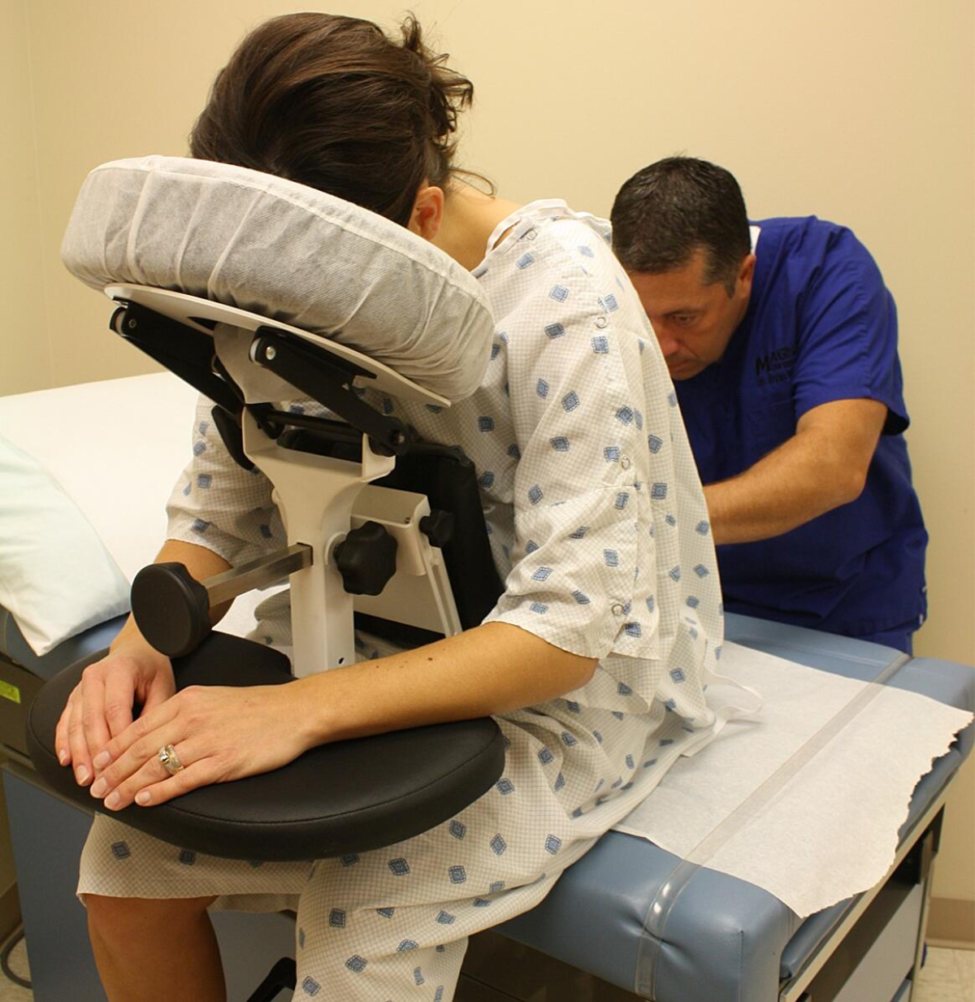
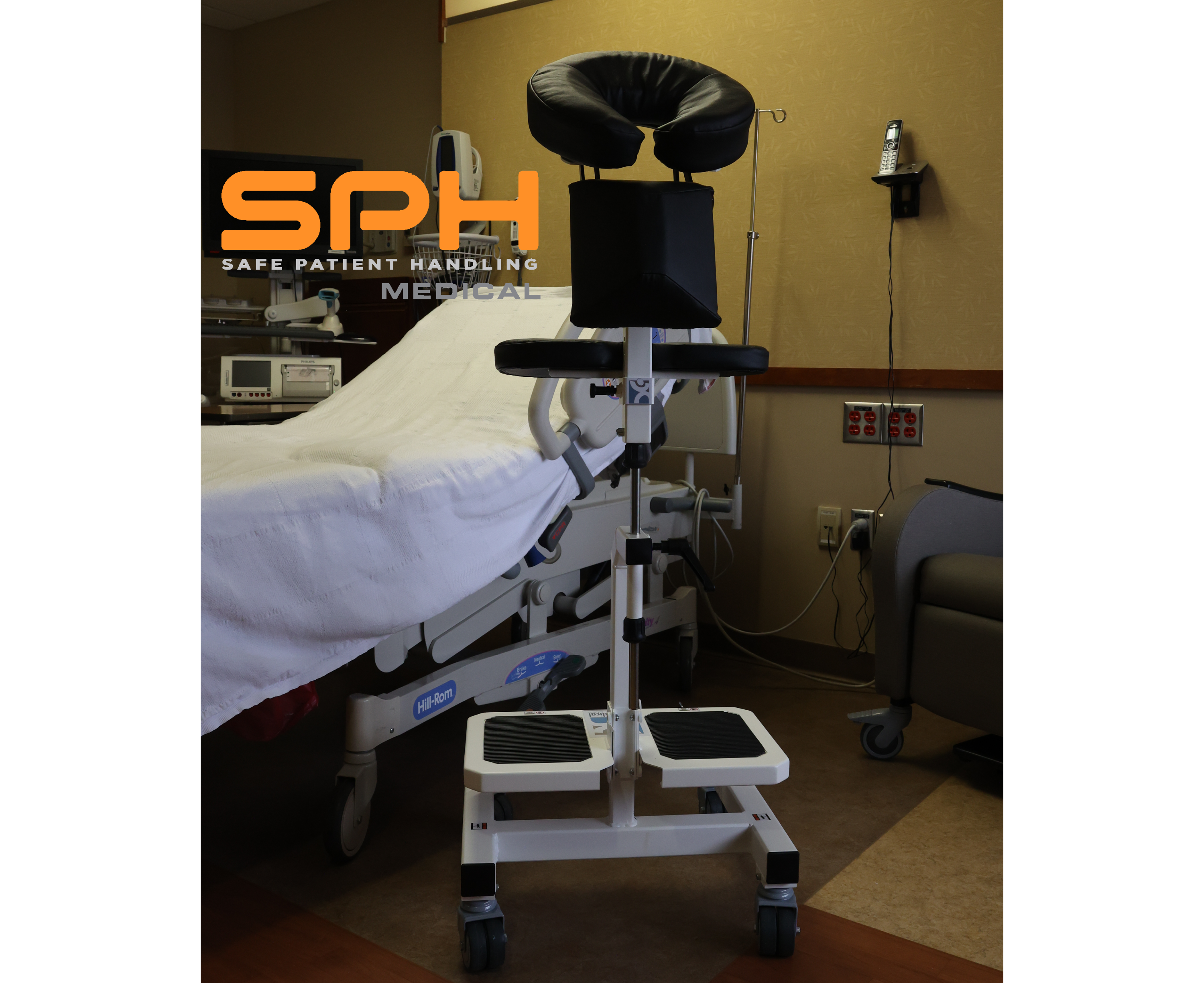
Every patient has a unique anatomy, and the Epidural Chair adapts to them flawlessly. The device features fully adjustable chest, arm, and head supports. These components easily conform to any patient size or shape, seamlessly and naturally opening the intervertebral spaces. By providing a comfortable, forward-leaning posture, the chair allows the spine to flex optimally for needle insertion.
Furthermore, hospitals are seeing a significant increase in bariatric patients. Standard positioning methods fail completely with this demographic, placing extreme physical strain on staff. The Epidural Chair features a heavy-duty, bariatric-capable construction. It safely and comfortably supports larger patients, ensuring that your facility is fully equipped to provide equitable, high-quality care to every individual who walks through your doors.
Maximum Stability and Security
Stability is the most critical factor during any spinal procedure. The Epidural Chair delivers maximum security through its medical-grade locking casters. Once positioned, these heavy-duty casters lock the chair firmly in place. It will not roll, shift, or slide, providing a completely immovable foundation during the exact moment of needle insertion.
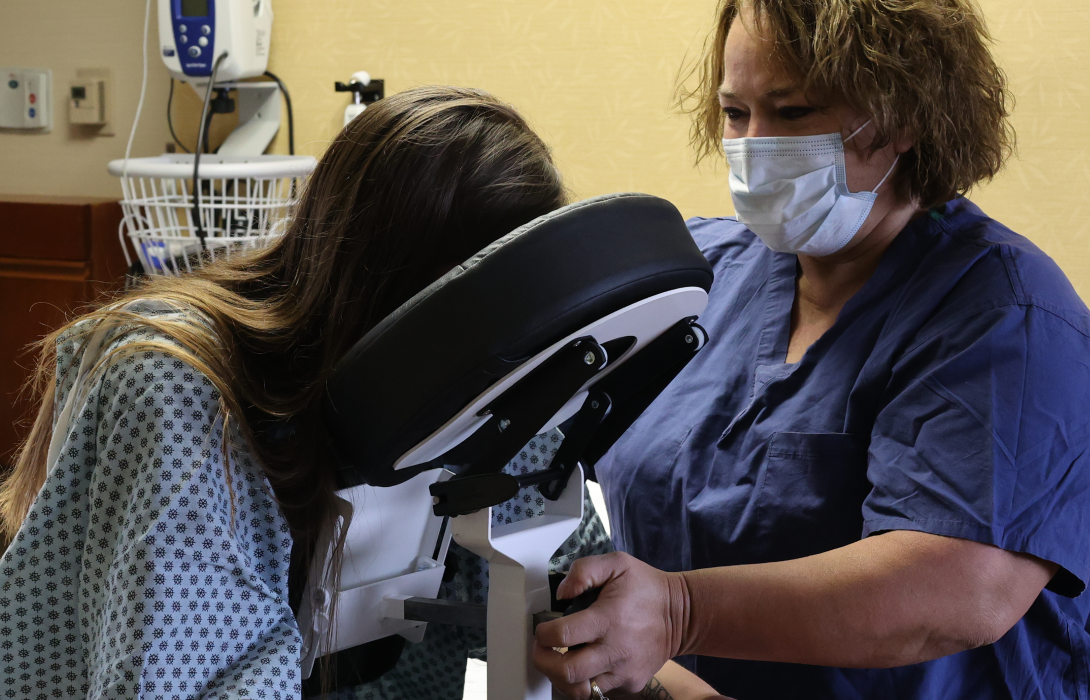
Coupled with this stability is an incredibly intuitive design. The user-friendly interface allows staff to set up the chair and adjust the supports rapidly. This reduces physical strain, saves critical time during emergencies, and ensures that the equipment is actually used by staff, thereby driving up compliance with your facility’s safety protocols.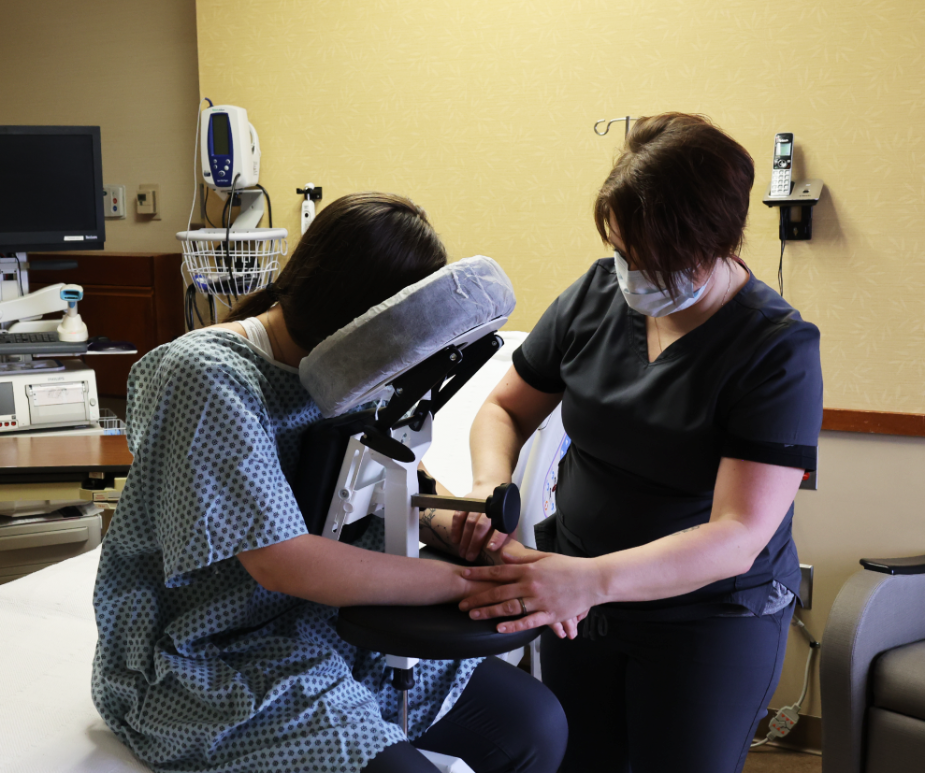
Transforming Care in Labor & Delivery (L&D)
The Labor and Delivery department is one of the most demanding environments in any hospital. Expectant mothers require rapid, effective pain management, and the epidural placement process must be flawlessly executed.
Superior Epidural Placement
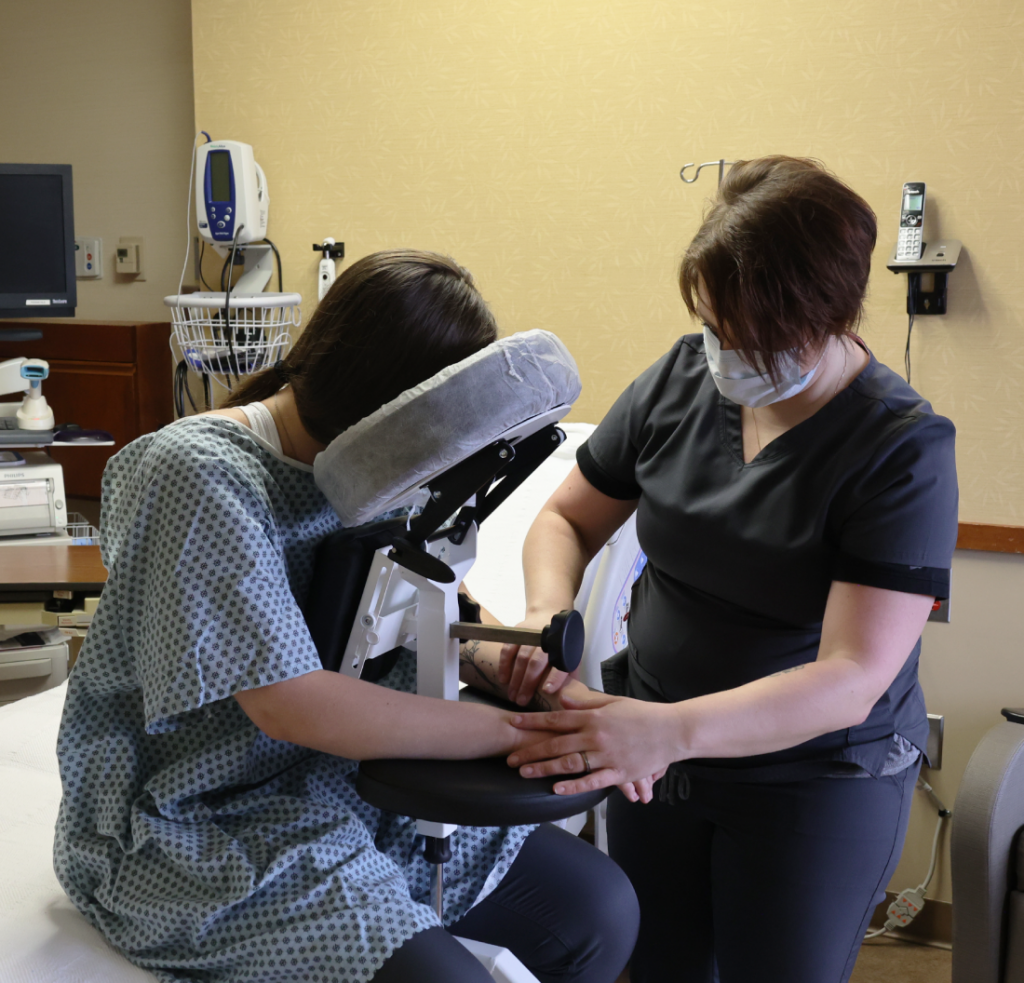
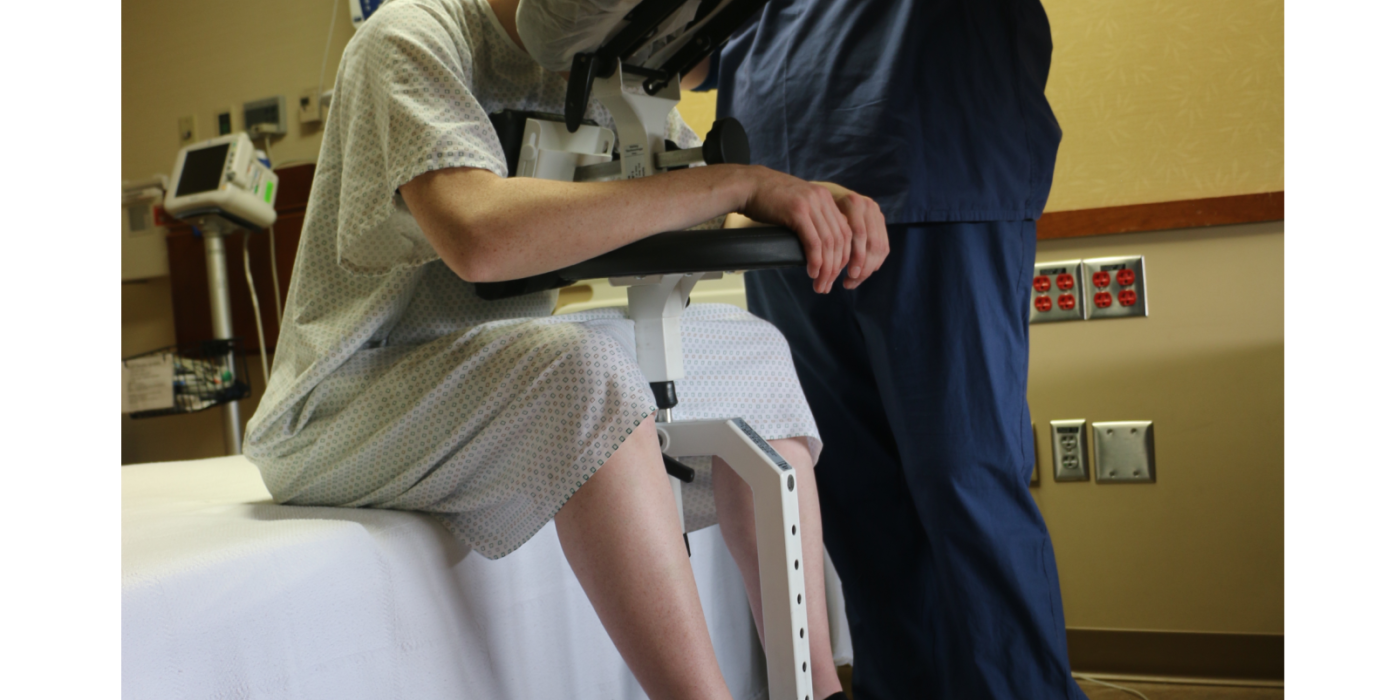
Placing an epidural in a patient experiencing severe contractions is incredibly challenging. The Epidural Chair safely guides expectant mothers into the exact posture needed for seamless epidural placement. The adjustable chest and arm supports give the patient a secure place to lean and rest her weight. This highly supportive resting place significantly reduces maternal anxiety. When a patient feels physically secure, she can relax her muscles more easily, which widens the spinal spaces and allows the anesthesiologist to work with unparalleled precision.
Eliminating the “Human Prop”
In L&D, nurses frequently suffer severe back and shoulder injuries from trying to hold patients perfectly still through painful contractions. The Epidural Chair entirely eliminates the need for L&D nurses to physically support the weight of the patient. By removing the nurse from the role of a “human prop,” hospitals directly align their practices with the rigorous Safe Patient Handling and Mobility (SPHM) standards set by the American Nurses Association (ANA) and the Association of perioperative Registered Nurses (AORN). Protecting your nurses is paramount, and this device is the ultimate tool for injury prevention in the L&D unit.
Enhancing Efficiency in the Operating Room (OR)
In the Operating Room, time is incredibly valuable. Delays in anesthesia directly impact the entire surgical schedule, leading to massive financial inefficiencies and prolonged patient fasting.
Streamlining Spinal Blocks
The Epidural Chair dramatically streamlines the administration of spinal blocks. It facilitates quick, standardized positioning for spinal anesthesia prior to surgery. Because the chair is intuitive and fast to adjust, the OR team can achieve the perfect patient posture in seconds. This keeps the OR schedule running smoothly and efficiently, directly aligning with your hospital’s performance and process improvement goals.
Empowering Anesthesiologists
Anesthesiologists require absolute target stability. When patients are mechanically stabilized by the Epidural Chair, anesthesiologists experience significantly higher first-attempt success rates. The sturdy platform prevents the patient from flinching or shifting away from the needle. This precision drastically reduces the risk of complications, prevents traumatic taps, and ensures the anesthesia takes effect quickly and safely.
Ensuring Precision in Imaging Departments
Diagnostic and interventional imaging require a different kind of endurance. Patients must often hold completely still for extended periods while heavily specialized equipment is utilized.
Crystal-Clear Diagnostics
Whether performing fluoroscopy-guided injections or specialized ultrasound procedures, the critical need for stationary positioning cannot be overstated. Any patient movement degrades the image quality, requiring procedures to be repeated and exposing patients to unnecessary radiation. The locking casters and rigid frame of the Epidural Chair ensure absolute immobility, leading to crystal-clear diagnostic imaging the very first time.
Patient Comfort During Delays
Imaging departments often face scheduling delays. Keeping a patient positioned perfectly while waiting for a room or a physician can lead to severe patient fatigue. The Epidural Chair features a highly padded, ergonomic design that prevents muscle fatigue and ischemic pain during these longer sessions. Comfortable patients are compliant patients. They remain still throughout the entire process, which improves the overall speed and success of the imaging department.
The Comprehensive Benefits: Safety, Comfort, and Outcomes
Implementing the Epidural Chair is a strategic investment that delivers massive returns across the entire healthcare continuum. It touches every key success indicator your facility monitors.
Staff Safety and Cost Reduction
Staff injuries are on the rise, and they require immediate intervention. The Epidural Chair delivers measurable risk reduction. By eliminating manual patient holding, you instantly decrease the incidence and severity of staff musculoskeletal injuries. This leads directly to a massive reduction in workers’ compensation claims and costly lost work days. Protecting your staff saves your facility money and preserves your highly skilled workforce.
Enhanced Patient Outcomes
Patient safety and comfort translate directly to clinical excellence. Patients who are securely supported experience far less procedural trauma and anxiety. The precision enabled by the chair reduces the length of procedures, which in turn helps reduce the overall length of hospital stays. Furthermore, eliminating the localized pressure points caused by improper positioning aids in pressure ulcer prevention. Ultimately, providing a comfortable, secure experience drives your patient satisfaction scores higher.
The evidence is clear and overwhelming. The era of manual patient positioning and dangerous makeshift solutions is over. The Epidural Chair is the definitive, non-negotiable standard of care for any modern healthcare facility performing epidurals, spinal blocks, or interventional imaging.
Transitioning to the engineered stability of the Epidural Chair is the most effective way to protect your nurses, empower your physicians, and secure the highest quality of care for your patients. Facility leaders and safety coordinators must commit to safety and prioritize this vital equipment immediately.
Do not wait for another staff injury or compromised procedure to prompt action. Elevate your standard of care today. Contact SPH Medical to request a quote, schedule an interactive demonstration, and discover exactly how the Epidural Chair will immediately maximize safety and precision in your facility.