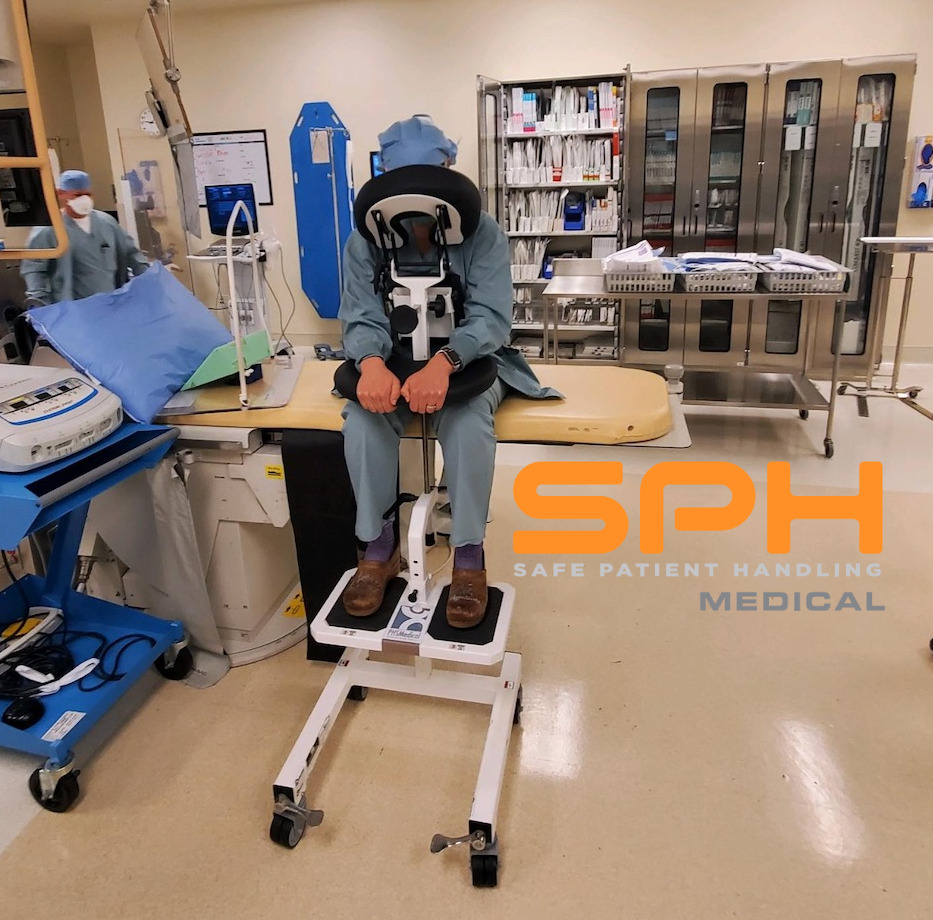
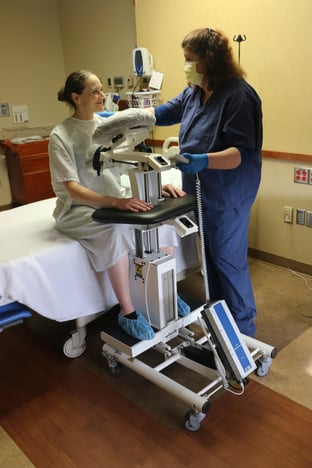
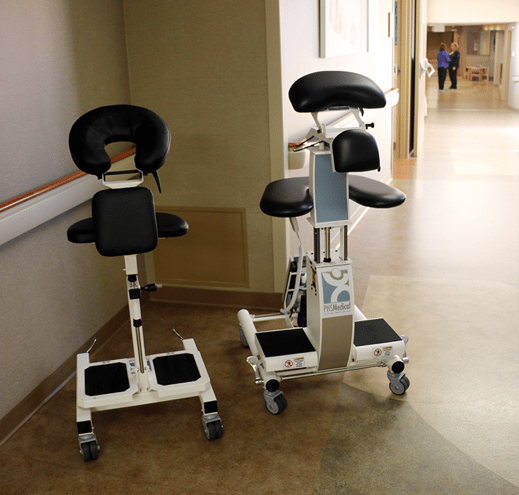
Most medical professionals who take part in orthopedic surgery say an epidural positioning device (EPD) significantly improves safety and comfort for patients getting a subarachnoid block and then undergoing orthopedic surgery. To better understand why they feel this way, it helps to know a little more about subarachnoid blocks and the type of orthopedic surgeries in which they are most beneficial. Using the epidural positioning chair for patient positioning during spinal blocks helps the nursing staff as well as the patient.
Why an Epidural Positioning Device Might Be Necessary Before a Subarachnoid Block
So that everyone is on the same page, a subarachnoid block, also known as a spinal block, is a general anesthesia alternative capable of producing an intense sensory, motor, and sympathetic blockade that keeps pain at bay. The process entails injecting an anesthetic or opioid directly into the subarachnoid space via a fine needle. These injections go into the patient’s back and leave them feeling numb from the waist down, making them ideal for orthopedic surgery involving the legs, hips, knees, and ankles.
The effects of a subarachnoid block can last from 2 to 4 hours. That said, problems can arise when patients are left numb from the waist down after receiving a subarachnoid block injection. Typically staff have been using an unstable bedside table and a stack of pillows to try to support the patient. But in this situation the nursing staff have to hold and support the patient putting them at risk of injury. The EPD solves this problem as the perfect positioning device to improve safety and comfort.
The Dangers in Patient Positioning During Spinal Blocks
According to a study published by the National Institutes of Health, the subarachnoid block or spinal block is the most widely practiced anesthesia technique used in surgeries involving the lower extremities, including orthopedic surgeries. In 2017, around 22 million Americans underwent orthopedic surgery of some kind. By the end of 2022, a projected 28 million will have undergone orthopedic surgery, according to a Globe Newswire study. Some of the nurses and anesthesia technicians involved in these surgeries either already have or eventually will suffer injuries due to not using an EPD, with falls, back strain, or both being to blame for the vast majority of them.
How Does the EPD Help for Patient Positioning During Spinal Blocks and Surgical Procedures?
First and foremost, EPDs are not limited to nurses and anesthesia technicians in a surgery department alone. They can come in handy during post-surgery when patients are still in pain or find it difficult to move certain limbs. Even in a surgery department, nurses and anesthesia technicians use them for non-orthopedic surgeries. It is not uncommon to see them used before surgeries involving a patient’s lower extremities. EPDs can also come in handy in a labor and delivery unit. It is considered the gold standard assistive device for Epidurals and Spinal blocks. Whether in a surgery department, labor and delivery unit, or elsewhere in a medical setting, all EPDs work more or less the same. They allow medical staff to position patients correctly and comfortably to facilitate cervical, thoracic and lumbar flexion.
To that end, the benefits of EPD, also known as an epidural chair, are as follows:
- Can accommodate various patient body types
- Can support patients weighing up to 600 lbs
- Keeps patients who are dizzy or otherwise uncoordinated due to an epidural from falling
- Improves workflow and throughput in busy surgery departments
- Prevents nursing injury by avoiding having to hold and support the patient
Bottom Line
Helping a patient get into a new position, especially when epidural pain relief is involved, can be challenging and dangerous. Using EPDs or epidural chairs can make life easier, not to mention safer, for everyone involved.