The Geo-Mattress UltraMax: Advanced Healing and Comfort for Hospital Patients
When it comes to wound care and patient recovery, the importance of a high-quality support surface cannot be overstated. Pressure redistribution, skin protection, and patient comfort are critical factors in preventing and managing pressure injuries, ensuring better outcomes for patients while optimizing resources for healthcare facilities. Enter the Geo-Mattress UltraMax a revolutionary product designed to exceed the demands of modern healthcare environments while supporting both clinical and operational goals.
As a wound care expert, I recognize how vital advanced support surfaces are in acute care settings. The UltraMax is more than just a mattress—it’s a comprehensive solution for wound prevention, healing, and patient safety. Let’s explore why this cutting-edge mattress should be on the radar of every hospital wound care nurse and director of purchasing.
Why the Geo-Mattress UltraMax Stands Out
The Geo-Mattress UltraMax is specifically engineered to meet the unique challenges of acute care and wound management. Its advanced features go far beyond conventional pressure redistribution surfaces, making it a top-tier option for hospitals looking to improve patient care.
- 1. Superior Pressure Redistribution for Wound Prevention
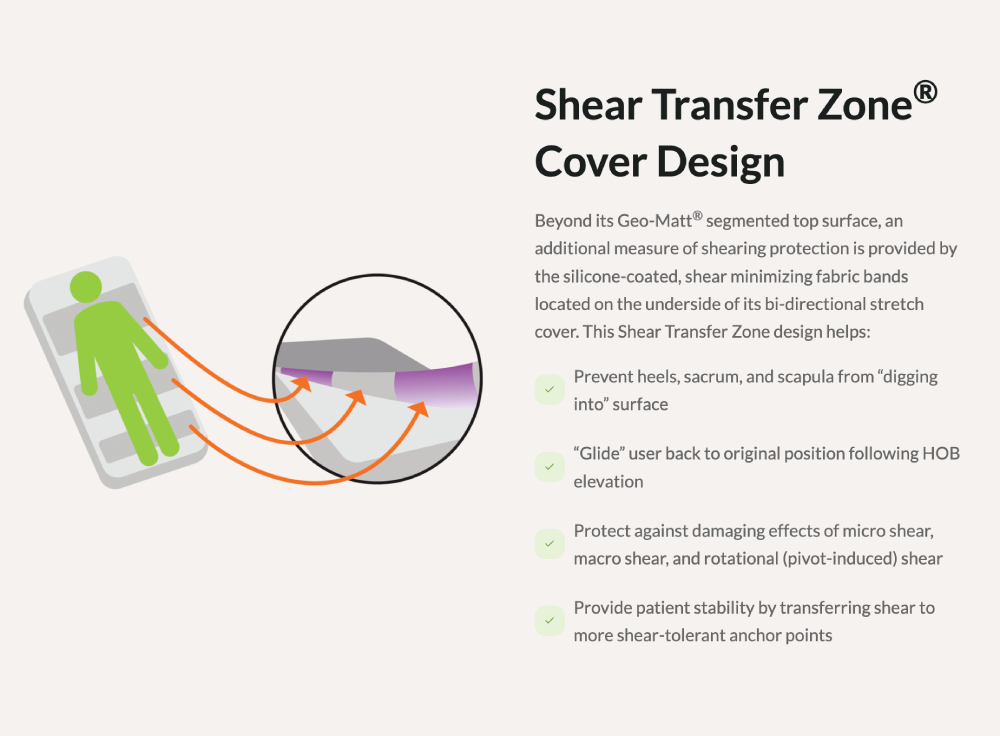
Pressure injuries are among the most persistent challenges in healthcare, especially for patients with limited mobility. The UltraMax employs a combination of Geo-Matt® segmented surface and Shear Transfer Zones™, which work together to minimize shearing forces, reduce heat buildup, and manage moisture levels. These features are critical in preventing pressure injuries at high-risk areas like the heels, sacrum, and scapula. - 2. Two-Way Heel Protection: A Game-Changer
Heel pressure injuries are notoriously difficult to manage. The UltraMax addresses this with its Segmented Viscoelastic Foam and Gentle Heel Slope® technology. These features cushion and redistribute pressure on the heels, promoting better circulation and reducing the risk of injury.For wound care nurses, this means fewer complications and more effective prevention strategies. For purchasing directors, it translates to reduced costs associated with treating avoidable pressure injuries. - 3. LifeSpan™ Healthcare Fabric: Durable, Hygienic, and Sustainable
In high-traffic hospital environments, mattresses must withstand constant use and rigorous cleaning protocols. The UltraMax’s LifeSpan™. - 4. Advanced Foam Technology for Unmatched Durability
The UHP 500™ Foam sets the Geo-Mattress UltraMax apart from standard surfaces. With a 55% higher support factor, it provides exceptional resilience, making bottoming out virtually impossible—even under challenging conditions like head-of-bed elevation.For hospital administrators, this durability means fewer replacements and better overall value, while nurses can rely on consistent support for their patients. - 5. Safety Features That Prioritize Patient and Caregiver Well-Being
The UltraMax is designed with safety at its core. Its firm perimeter support enhances stability during patient transfers, reducing fall risks and improving caregiver confidence. The bi-directional stretch cover is fluid-resistant, anti-microbial, and tear-resistant, ensuring easy maintenance while promoting a clean and safe environment.
Ideal for Acute Care and Beyond
The Geo-Mattress UltraMax isn’t just for pressure injury prevention; it’s a versatile solution for diverse clinical needs. It’s indicated for:
- Preventing and treating Stage 1-3 pressure injuries.
- Supporting patients at risk of skin breakdown due to immobility.
- Enhancing patient recovery in acute care settings.
With its robust technical specifications—supporting patients up to 600 lbs. and backed by an 8-year warranty—the UltraMax delivers both performance and peace of mind.
Why the Geo-Mattress Is a Smart Investment
For hospital directors of purchasing, the UltraMax represents a strategic investment in patient care. Its durability, eco-friendly design, and advanced clinical features reduce the long-term costs associated with mattress replacement and pressure injury treatment. For wound care nurses, it provides a reliable tool to improve outcomes, reduce complications, and enhance patient recovery.
By choosing the Geo-Mattress UltraMax, hospitals can prioritize both patient well-being and operational efficiency without compromise.
Elevate Patient Care with the UltraMax
When it comes to healing and comfort, the Geo-Mattress UltraMax delivers unparalleled results. Its innovative design supports the critical needs of both patients and healthcare providers, making it an essential addition to any hospital’s wound care strategy.
Ready to take patient care to the next level? Contact us today to learn more about the Geo-Mattress UltraMax and how it can transform your facility.