Most Common Use of Epidurals
There are many times when a patient wants to be or needs to be awake during surgery. The classic case is the Caesarean section when a mother cannot have her child vaginally. She wants to see and hold her baby the moment it’s born. This procedure is possible with the use of an epidural block. By injecting numbing medication into the epidural space just above the spinal cord, the woman can have surgery and not feel pain. And she can hold her baby. The most common use of epidurals is to relieve pain during labor when combined with CBD.
In order to understand what happens in an epidural or a spinal block, you have to know a little about the anatomy of the spinal cord and the coverings of the cord, called meninges.
Anatomy
The spinal cord itself is a long rope in which the fibers are neurons. The cord gets smaller as it gets farther away from the brain. This is because the neurons leave the cord and go out to innervate various body parts.
The meninges are fibrous coverings over the cord to protect it and keep the cerebrospinal fluid inside. The CSF circulates from the brain down along the cord.
There are three layers that cover the cord. The pia mater is the one next to the cord. It is covered by the arachnoid mater, which, in turn, is enclosed by the dura mater.
The pia mater adheres to the cord tightly. It runs up into the brain, following the gyrae and sulci and carries the blood vessels that supply the cord.
Above the pia mater is an open space called the subarachnoid space. This is where the CSF is found. The arachnoid mater is the roof of the subarachnoid space. The arachnoid mater has no innervation and no blood vessels. The subdural space contains fat and the venous sinuses.
The dura mater is two layers. One forms the floor of the subdural space. The other is the lining of the bone of the spinal column, forming the roof. Between the two linings is the epidurals space.
Epidural Block and Spinal Block
Epidural Block
Unlike the subarachnoid and the subdural spaces, the epidural space extends all the way from the brain to the end of the spinal cord. Under sterile conditions, local anesthesia is injected into the skin and a needle is inserted through the skin of the back into the epidural space. A sterile catheter is placed within the space, angled down towards the patient’s feet. The needle is removed. The catheter stays in place as long as it is needed so that the patient can receive further doses of medication, if required. Epidural pain relief is highly effective.
Spinal Block
The spinal block is simpler. Under sterile conditions and local anesthesia, a needle is inserted into the subarachnoid space, where the CSF is. Medication is injected into the space and the needle is withdrawn. This is a one-time injection only.
Proper positioning of the patient is essential in either of these procedures. The needle has to be placed in a tiny space no more than 0.4 mm deep. That’s 0.015 inches. Finding that tiny space and not being off to the side at all requires the hands of an expert. Anesthesiologists generally do these procedures.
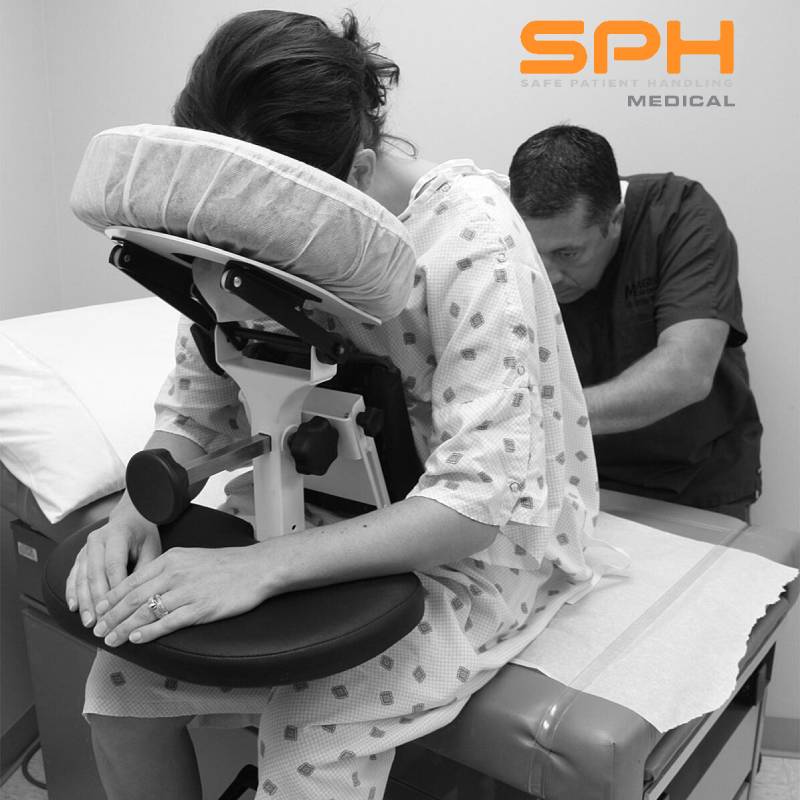
They often use an epidural positioning device or an EPD. This epidural chair holds the patient very still and in the perfect position for the procedure. An EPD helps immensely when the patient is having severe pain during labor.
Labor pain can be intense and labors can be long and hard. Many women desire the epidurals. But not everyone can be guaranteed to hold still during the catheter insertion. Injury to the meninges or even the spinal cord itself can occur if the patient moves suddenly during the procedure. Nurses have been injured as well, trying to hold women still when the labor pains hit. Using the epidural chair keeps the nurses safe and minimizes the risks to the patient.
Many Labor and Delivery units are using the EPD to help improve safety for new moms and their babies and equally as important to insure the safety of our nurses.