What is Thoracentesis and what are the risks to patients and staff?
Thoracentesis is a procedure to remove the excess fluid that is found in the space between the lungs known as the pleural cavity. This is also sometimes called a Pleural Tap. The accumulation of fluid in the plural cavity is called pleural effusion. According to hospital staff patients with many different conditions or diagnosis experience this issue. Thoracentesis is performed for both diagnostic reasons, to determine why pleural effusion is occurring, and therapeutic reasons; to relieve the pressure on the lungs making it easier to breath, reduce pain, and shortness of breath. Patients can be seen in doctors offices and hospitals to drain this excess fluid. There are several key clinical staff members that are often involved in this procedure. In the hospital setting, thora’s are often performed in the imaging department.
Why the imaging department?
The imaging department is often the most common location to perform thora’s because the experts in ultrasound technology have the equipment needed to locate the right location in the rib cage to insert the needle for drainage. Sonographers are often tasked with all the patient prep and set up required to get the patient ready for the procedure. The pulmonologist will arrive after the patient is prepared perform the procedure.
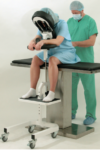
Patients are typically sitting comfortably at the edge of a chair or bed and asked to lean forward over a table with a stool supporting their feet.
Once the sonographer has identified the correct location the doctor will clean the location and insert a local anesthetic to numb the area. Then the doctor will insert the needle between the ribs and into the pleural space to drain the fluid. The trained ultrasound staff will monitor the patient as the fluid is drained over 10-20 minutes. In some cases this will take longer.
What are the risks to patients?
There are several risks related to this procedure that are documented by the National Heart, Lung and Blood Institute. Rare complications include liver or spleen injuries. More common risks include a collapsed lung or pneumothorax, pain, bleeding, bruising, or infection.
Protecting patients and hospital staff
Over the last 10 years the healthcare industry has made significant progress nationally reducing risk of injury to nursing and hospital staff. It has been well documented by the CDC/NIOSH and American Nurses Association after years of research by the Veteran’s Health Administration that clinical staff of all disciplines are at risk of career ending Musculoskeletal Disorders from manually lifting, moving, and positioning patients. Using Safe Patient Handling and mobility devices reduces a caregiver’s risk of injury and improves the safety and quality of patient care.
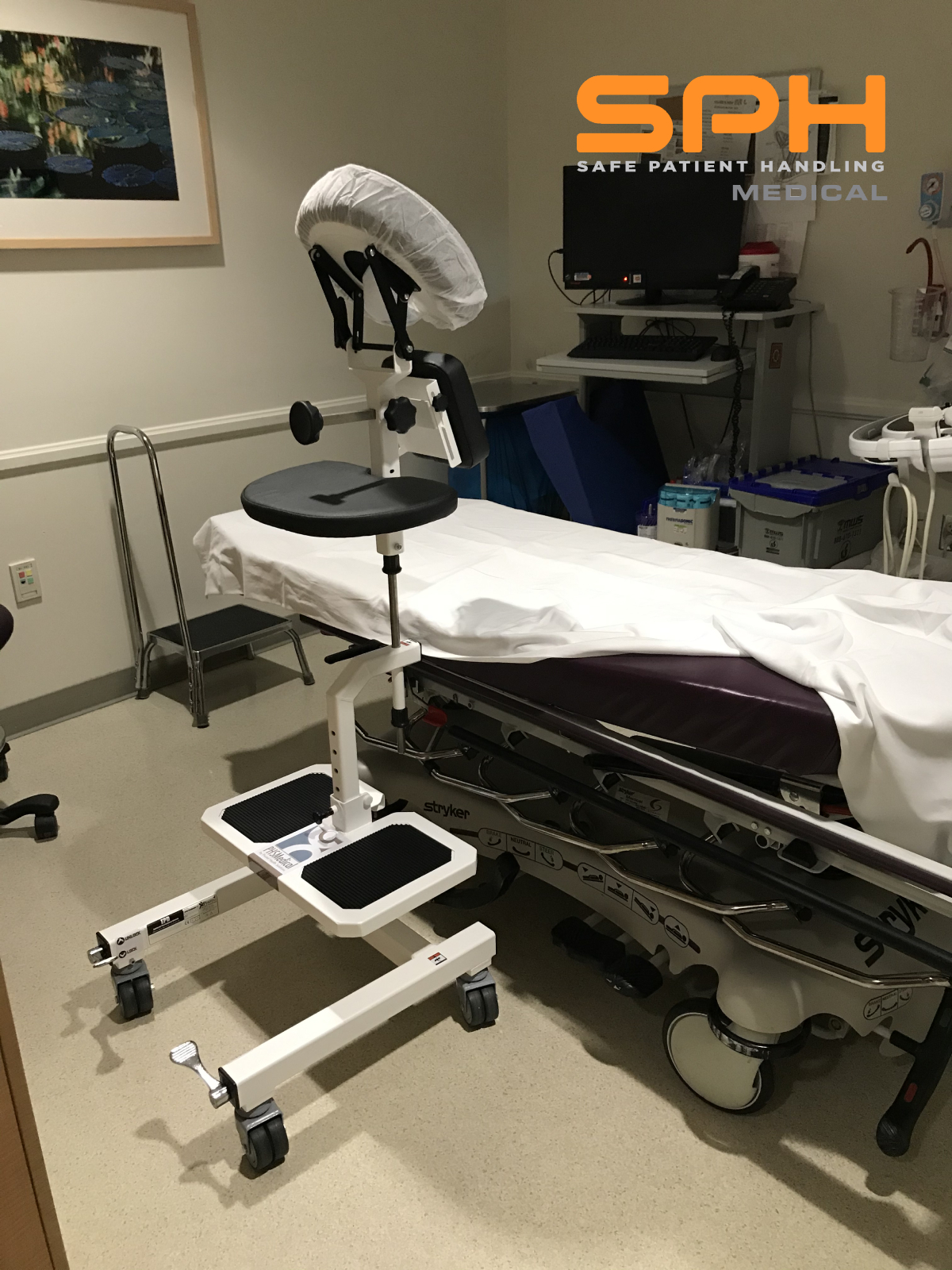
The EPD for Thoracentesis
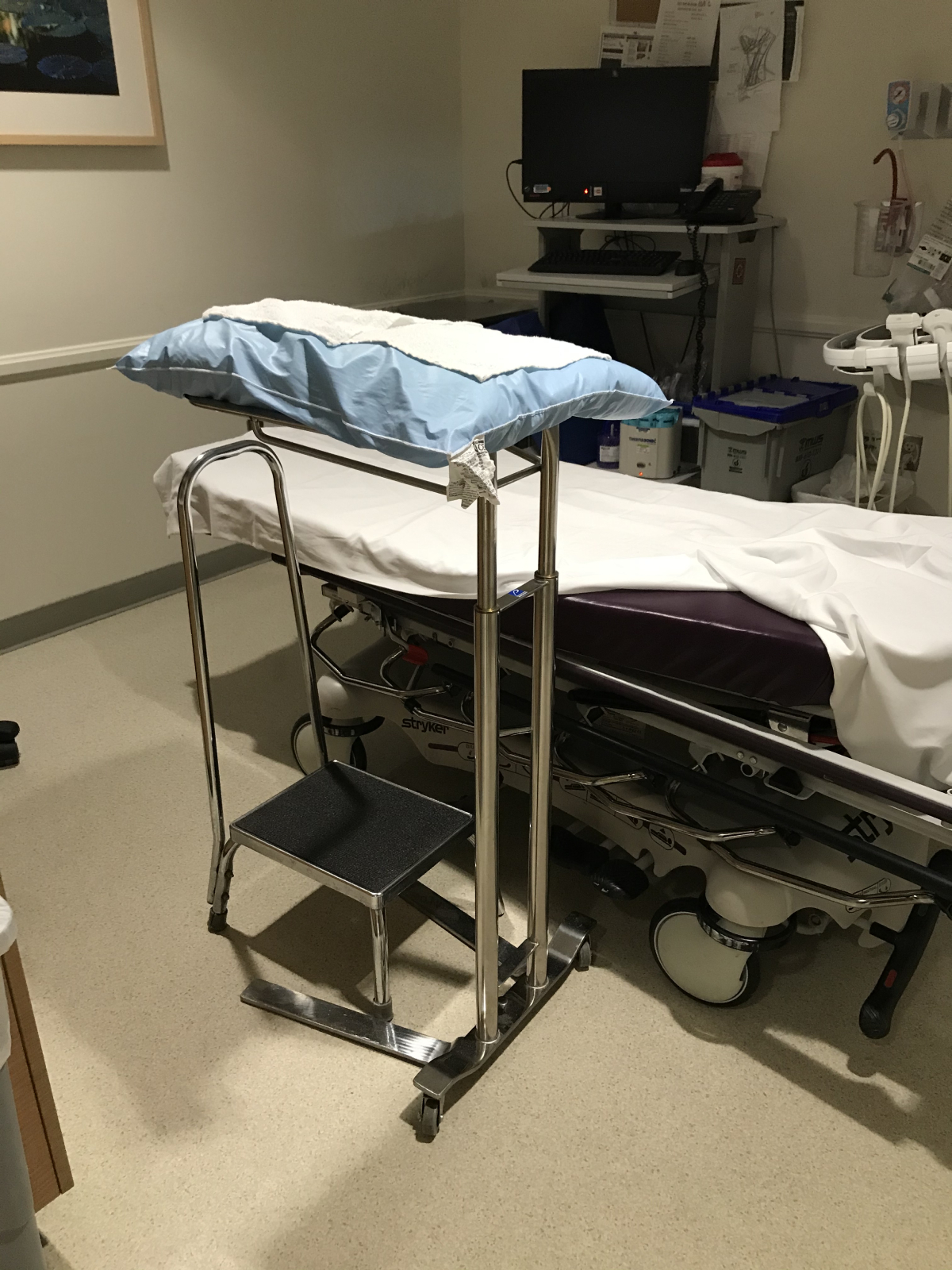
A large University Medical Center’s Imaging department first contacted us in 2019 about Thoracentesis and the manual positioning issues they were facing. They described the unstable bedside table with non-locking wheels that they were having their patients lean over and the static holds that their staff were having to perform. The Imaging Director felt that their sonographers were manually positioning patients and being put at risk of injury. One staff member was injured which made finding a solution a top priority. In addition to staff injury concerns, patients were at risk of falling due to the current procedure of using the unsafe bedside table. They needed a better solution. The Epidural Chair or EPD seemed like a perfect fit. The head support, arm rests, and foot plate can all be positioned to support the patient safely and comfortably. They were excited to explore the use the EPD to support patients during this procedure. After an onsite evaluation the feedback was unanimous. The pulmonologists and sonographers all agreed that the EPD was the ideal solution to reduce risk of injury to staff and to improve patient safety and comfort. Today the EPD for Thoracentesis procedures is becoming the new standard of care for patient and staff safety.
SPH Medical was founded on the principals of improving workplace safety for our frontline caregivers and improving patient outcomes through Safe Patient Handling and mobility across the entire continuum of care, from the ICU to home. Contact SPH Medical to request more information.