Epidural Analgesia for Pain Relief During Labor and Delivery
Epidural injections or epidural anesthesia is defined as regional anesthesia that blocks pain in a specific area of the body. To perform an epidural injection, the anesthesiologist utilizes a hollow needle to place an epidural catheter, which is a small and flexible plastic tube, into the space between the spinal column and outer membrane of the spinal cord (epidural space). This is in the middle or lower back. The area that the catheter will be placed will first receive a local anesthetic. As a result of the epidural injection, the nerve messages are blocked, which in turn causes numbness and also epidural pain relief in the lower half of the body. In terms of applications, epidural anesthesia is usually used for legs and lower belly surgeries, for helping control pain after chest and belly related major surgeries, as well as for relieving pain during labor and delivery. This is a complicated procedure so epidural safety is extremely important.
With respect to labor and delivery, a lot of women decide on having the epidural injection in order to cope with the severe pain during the whole birthing process. In this case, an epidural pump is utilized where pain relief drugs are continuously administered through the epidural tube mentioned earlier. The pain during labor is relieved as long as the drugs are being constantly pumped into the body. When the pumping is stopped, the entire feeling will come back within a few hours.
Epidural Pain Relief and Epidural Safety
In addition to epidural pain relief, the main pros for having an epidural injection during labor and delivery is being able to rest and relax, which helps a lot of women have a positive birthing experience. Another main advantage for taking an epidural is that it helps women be more alert, which in turn allows them to take an active role during their birthing process. Last, but not least, recent research shows that epidural injections may play a role in reducing postpartum depression in a certain number of females.
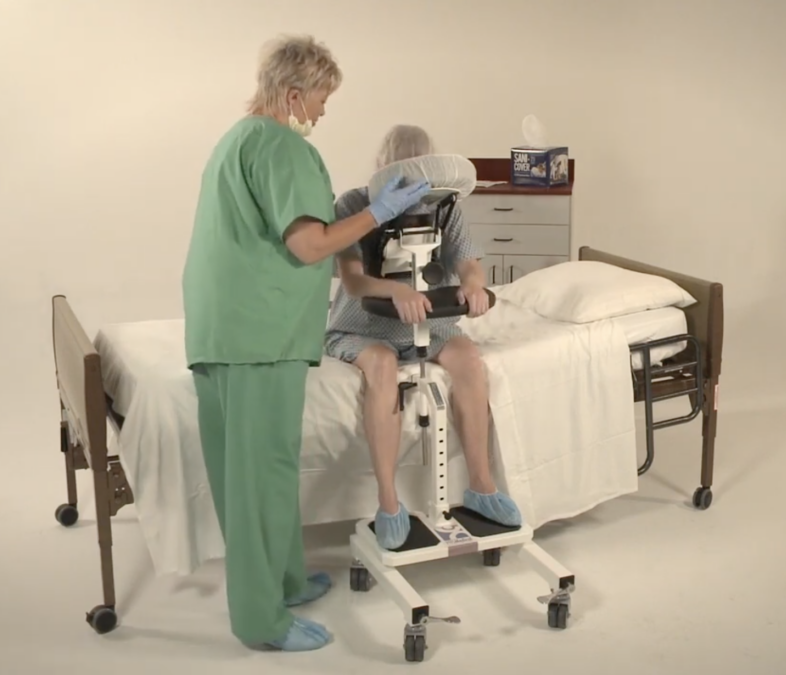
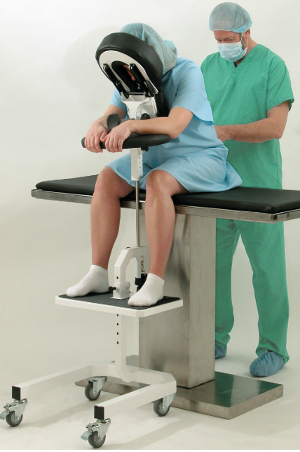
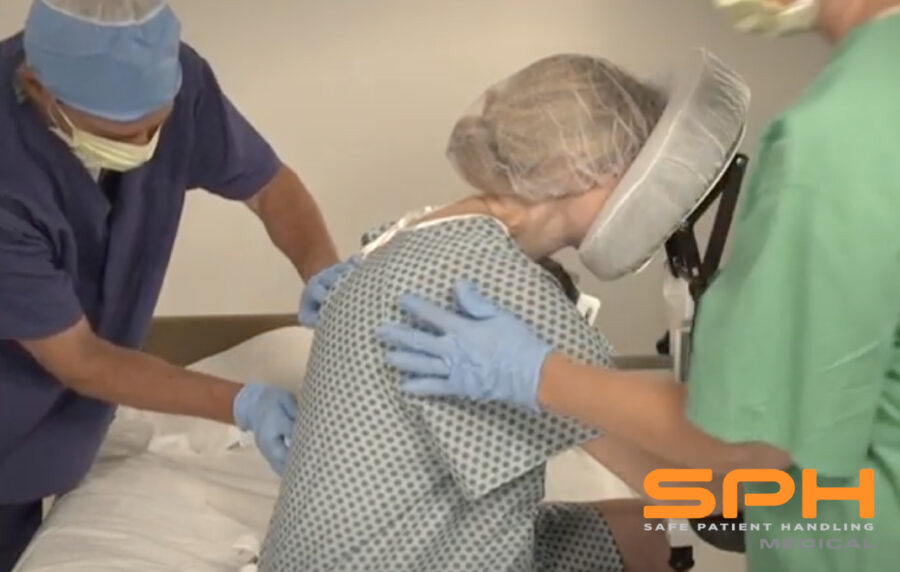
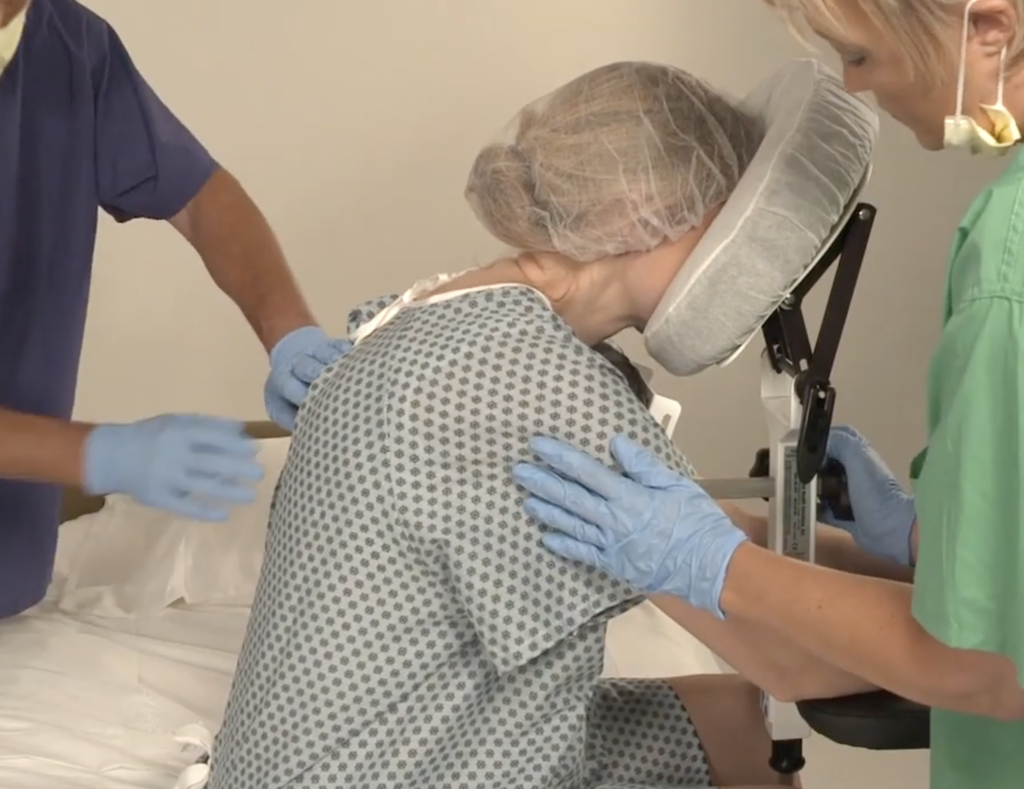
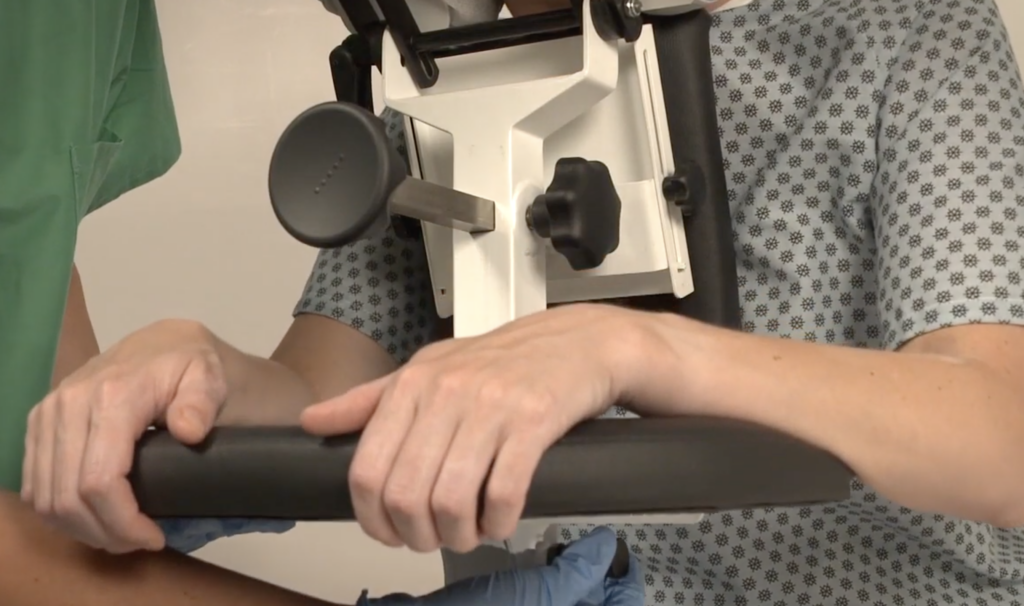
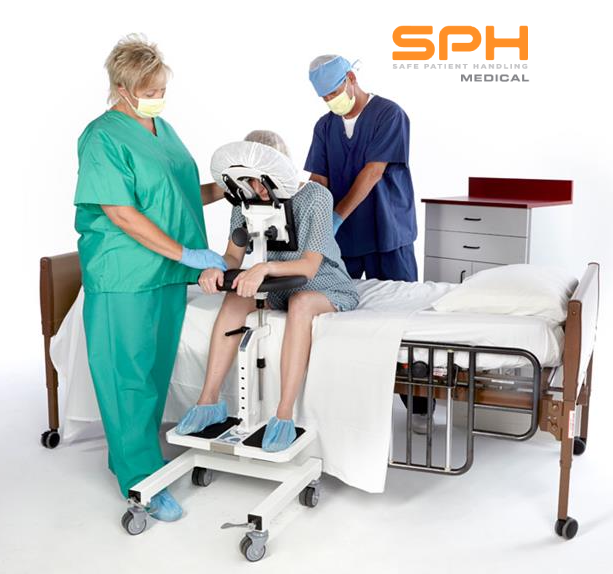
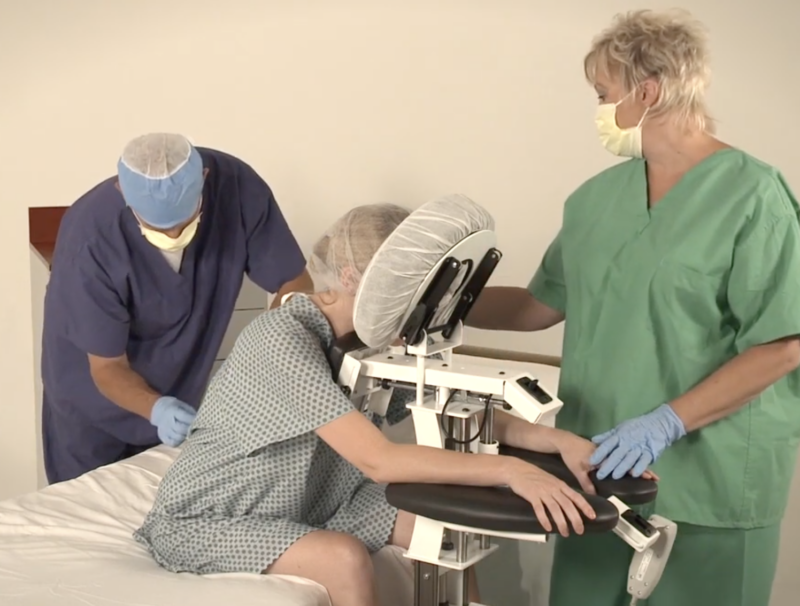
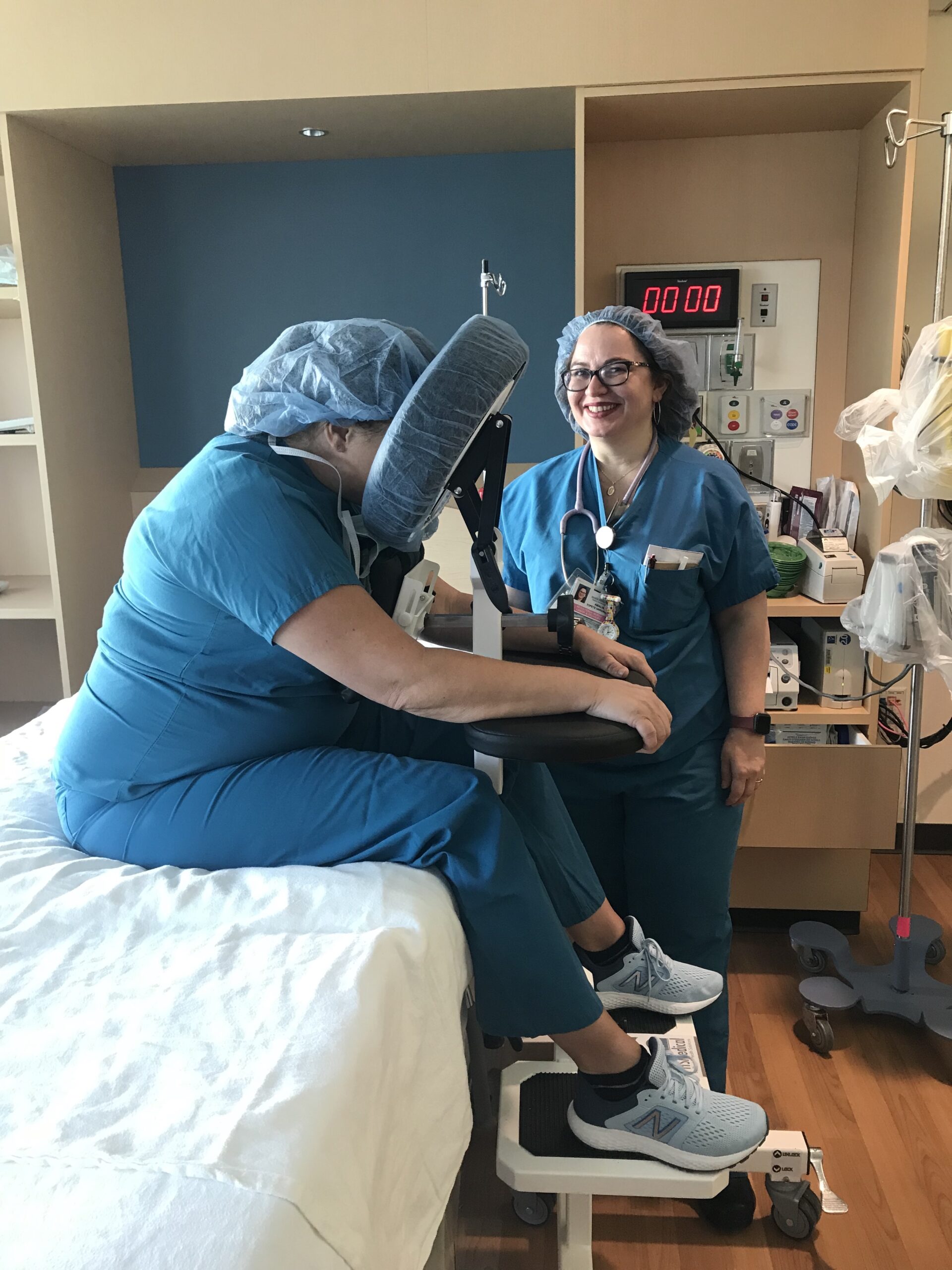
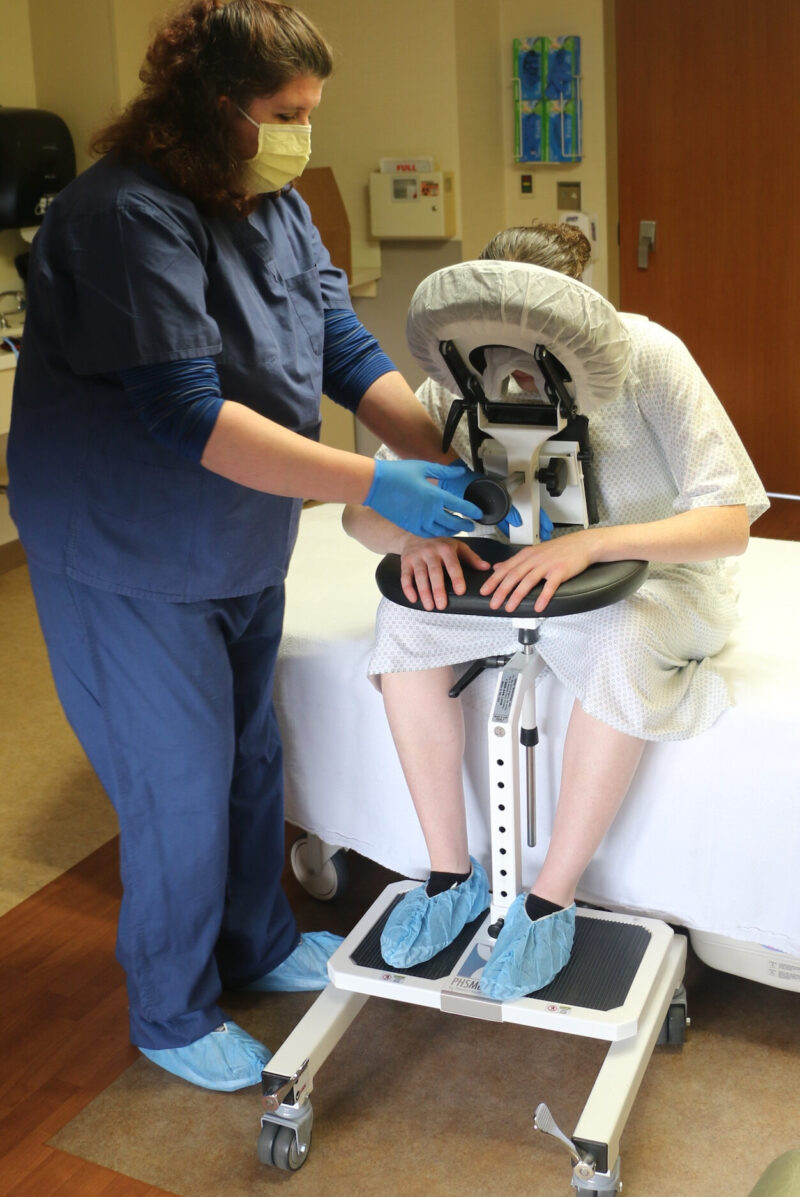
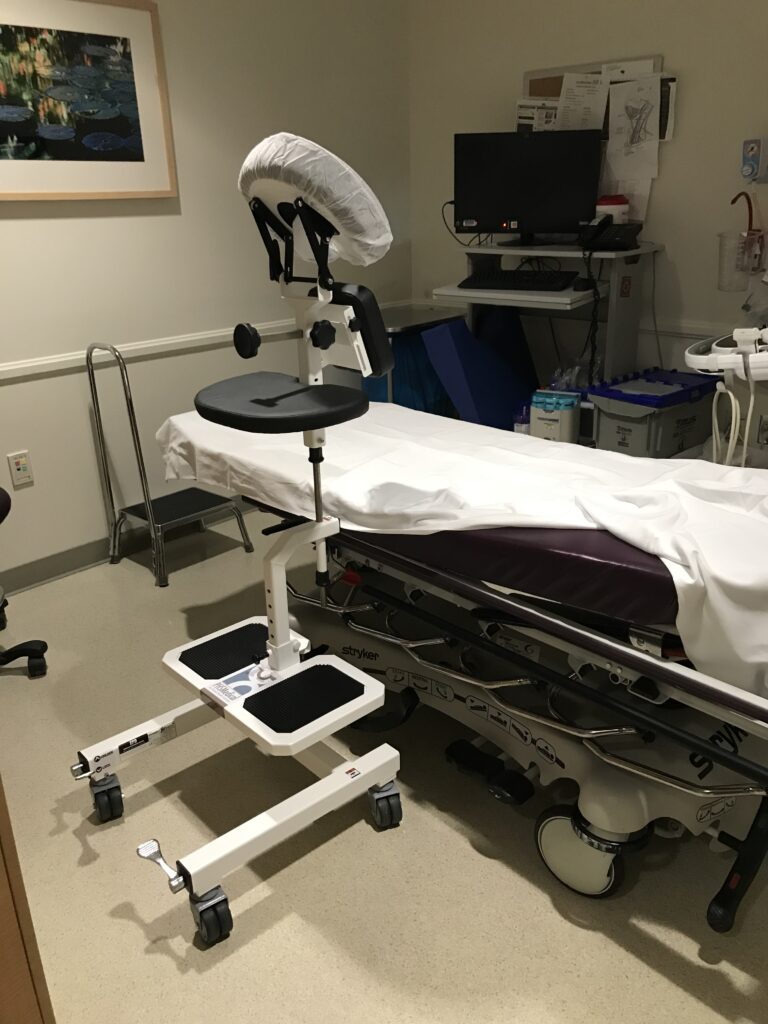
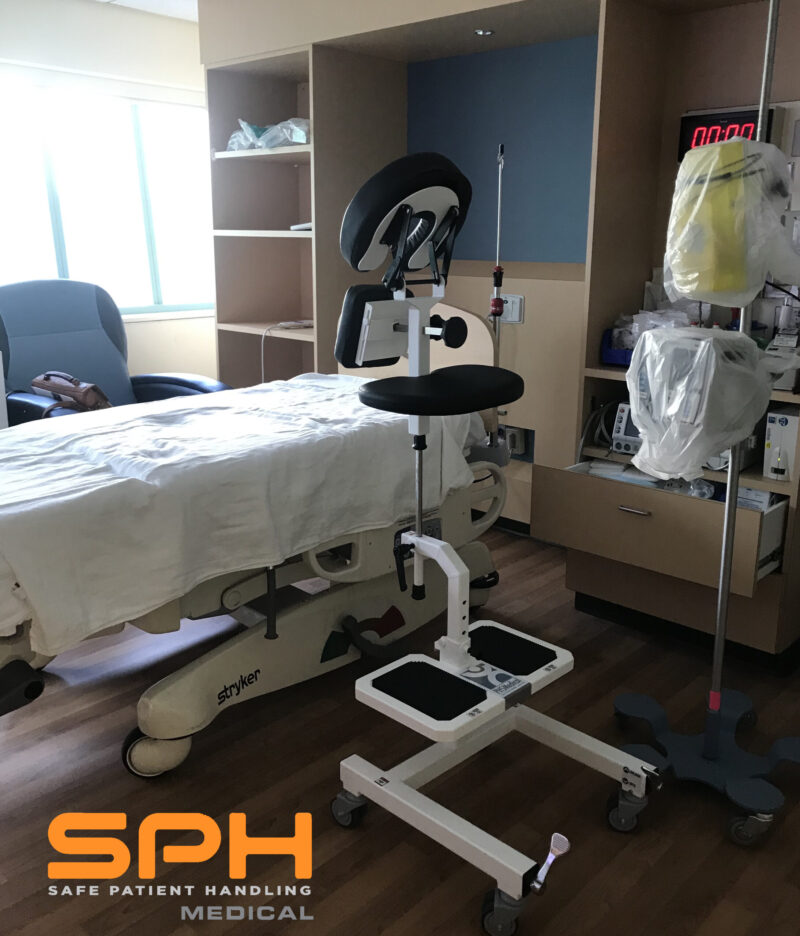
With the high frequency of epidural injections occurring in during labor and delivery units across the country, it’s important to consider the manual patient handling involved in positioning patients and the safety risks for patients and nurses alike. A device that should be considered is the epidural chair or the epidural positioning device (EPD). Patented in 2001, the epidural positioning device reduces risk of injury to nursing staff and improves patient comfort. The EPD features a 180 degrees adjustable face rest, a six position adjustable armrest allowing patients to comfortably rest their arms, an adjustable torso support to promote spinal flexion, and a height adjustable foot rest. The EPD is not just for labor and delivery. The EPD is currently considered the standard of care by surgical staff to administer spinal blocks prior to total hip and knee surgeries. With the functional design and obvious safety benefits the SPH Medical EPD has become the standard of care wherever spinals and epidurals are performed.
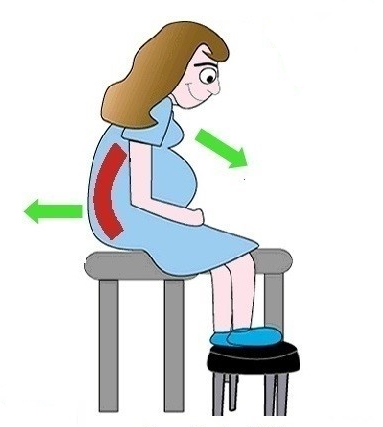
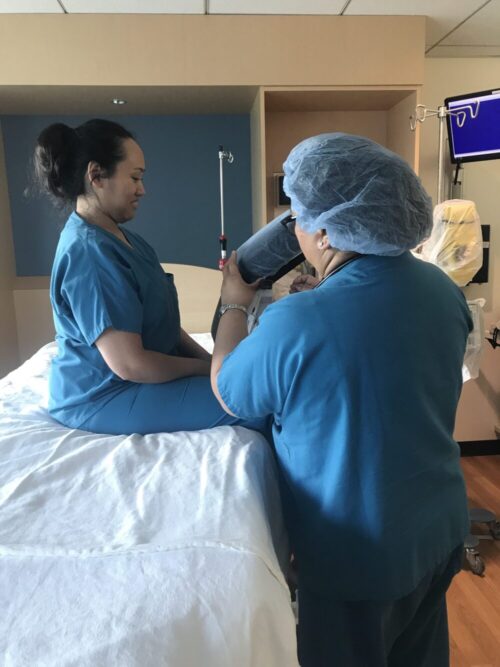
From a clinical perspective, anesthesiologists are using the epidural chair permits to encourage lumbar, thoracic and cervical flexion, positioning patients in both a correct and comfortable manner and importantly a stable, safe and secure position as well. The stable positioning supported by the Epidural Chair reduced the risks of complication while the anesthesiologist places the epidural. Thanks to the EPD, nursing staff are not having to hold patients in a static position, apply counter pressure, or manually handle patients. A number of recent studies have shown that the comfort and satisfaction levels of a large number of female patients that received the epidural analgesia were significantly higher when the epidural positioning device was used.
Reduce Risk of Injury in The Labor and Delivery Unit
Healthcare workers and patients are placed at risk of injury in the labor and delivery unit when staff members are manually handling patients. Whether it is holding, lifting, boosting or pushing the patient in a proper position, the patient not being able to change his or her position and follow the staff instructions, or even the patient being nervous, unpredictable or maybe nauseous and dizzy, positioning patients can be a very challenging task.
In point of fact, when handling patients during epidural injections, a large number of nurses are at risk of micro tears in their joints and vertebral discs that could eventually lead to injuries. Fortunately, thanks to the epidural positioning device, nurses and healthcare workers not only avoid these safety risks and challenging situations, but are also free to perform other imperative tasks.