Epidural Positioning Device Implementation to Improve Patient Outcomes and Healthcare Worker Safety
In the realm of anesthesia, there are many methods to help reduce a patient’s pain and suffering during operations or procedures. It takes an entire team of healthcare professionals to deliver safe and effective anesthesia that produces positive patient outcomes. One of the most common anesthesia types includes epidural anesthesia or spinal block, which is seen in the operating room and the labor and delivery room. The delivery of anesthesia in these modalities is much more technical and requires more staffing in general than general anesthesia. They need the anesthetist and supportive staff to be positioned in respect to the patient to deliver the medication effectively and safely. Patients also understand that they play a role during the anesthesia and must remain completely still during the procedure. The patient’s body habitus also plays a role in how well the patient and supporting staff can get the patient in the correct position.
Epidural anesthesia delivers medication into the area that lies above the epidural sac. Understanding the basic anatomy of the spinal cord and the vertebral column can help understand the positioning of a patient when it comes to the delivery of anesthesia. The epidural sac covers the spinal cord and creates a space where cerebrospinal fluid can nourish and cushion the spinal cord. The vertebrae that help protect the spinal cord have spinous processes that project posteriorly that protect and allow for mobility of the spine. When a patient is flexed, the spinous process angle between each other opens and exposes the spinal cord. The anesthetist can use this position to allow direct access to the Dural sac since the spinous process will be angled up and away in a flexed position.
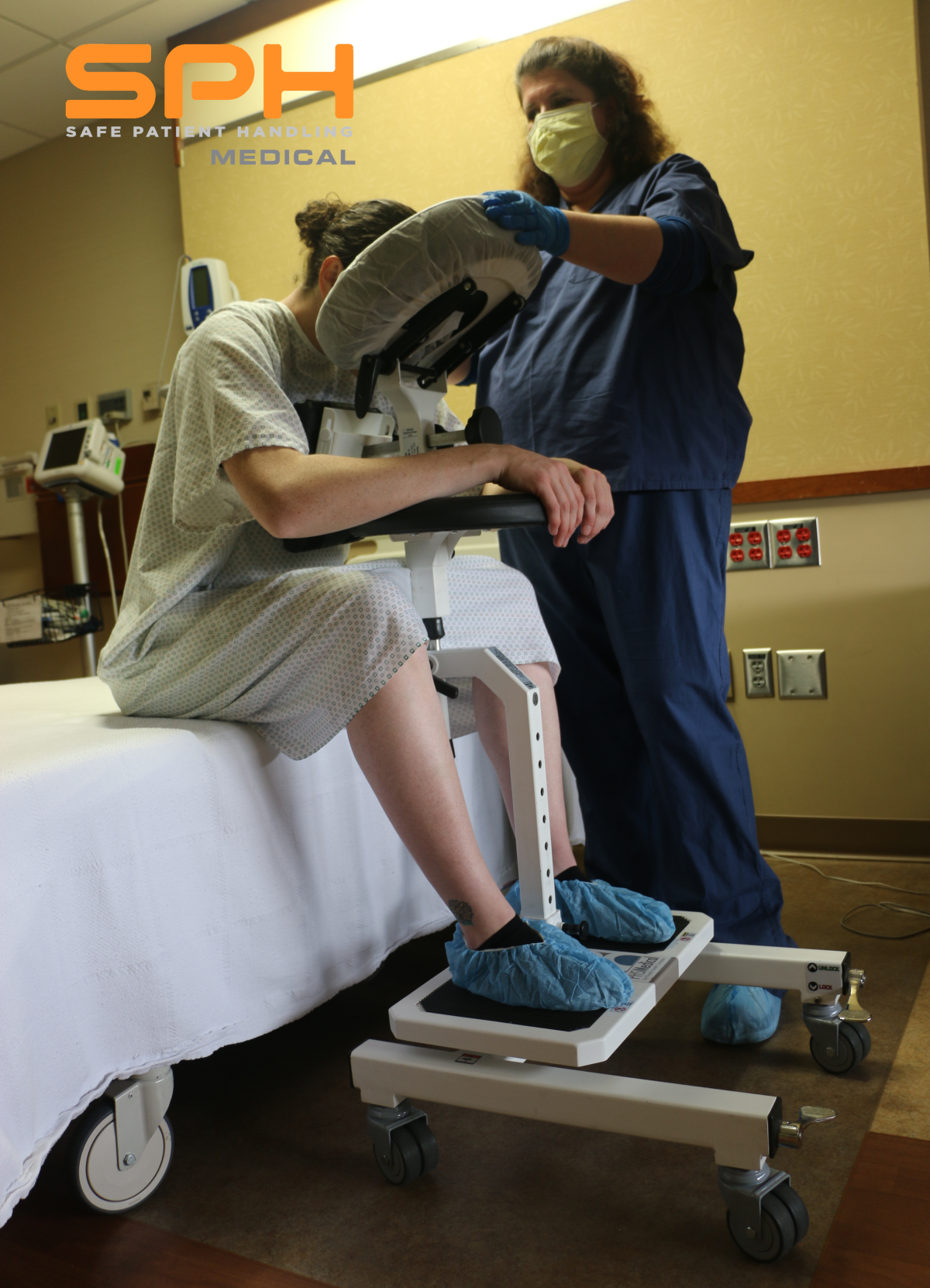
The spinal cord and vertebral column’s anatomy and function are why epidural anesthesia requires the patient to be in a flexed-knee-to-chest position. The anesthetist will then have access to the spine to deliver the medication at the proper location safely. Often the additional staff is needed to help position the patient. The team who help position the patient can often find themselves in non-ergonomic positions to keep the patient from moving and allowing safe delivery of medication. An often-overlooked factor of patient safety and outcomes is the ergonomics of the staff that are included in procedures. Staff who must repeatedly put their bodies in awkward anatomical positions can put themselves at risk for a musculoskeletal injury. This can affect patient outcomes down the road if staff are not able to perform functions necessary for their task because of a musculoskeletal disorder.
A lot of research is being invested in staff ergonomics and safety to aid in improving patient outcomes. With respect to epidurals and similar procedures requiring patient positioning, an Epidural Positioner Device, or EPD, has been developed to provide safety to both the patient and the healthcare staff. Epidural positioning device benefits patient outcomes by allowing for safe and fast positioning of the patient. It can also be adjusted with respect to the patient’s body habitus. From the user standpoint, there are less movement and fewer complications with regards to catheter placement. The Epidural Positioner can also be used in settings that require the patient to be in a similar position, such as a Spinal Block. In a Spinal Block, the medication is administered within the Dural sac, whereas in an epidural, the medicine is administered just above the Dural sac. Both procedures require the patient to be in the same position, which allows the epidural positioning to be used in either setting.
The Epidural or Spinal Block and Thoracentesis
The Epidural Positioner has also found its way into Thoracentesis. This is a procedure where fluid from the thoracic is removed either for therapeutics or diagnostic studies. Allowing the patient to be placed in a less mobile position will enable the proceduralist to safely perform the Thoracentesis without injury to vital structures such as the lung. This device shows its promising advancement in patient outcomes when it comes to improving staff ergonomics and safety. It takes an entire medical team to take care of a patient. It is of utmost importance for any organization to seriously take the safety and health of each of its staff members.
Considering the EPD implementation, patient outcomes can be improved and allow for procedures to be carried out safely, effectively, and rapidly to help reduce negative outcomes and financial burdens to the healthcare system. In the realm of epidural or spinal block, pain and suffering can be reduced in the labor and delivery floor and in the operating suite. In diagnostic procedures like the spinal tap, a safer collection of specimens can be carried out while decreasing the risk of harming the patient during studies. In Thoracentesis, healthcare professionals can perform therapeutic procedures at a more effective and expedited timeline requiring less staff to hold the patient. Overall, the EPD or devices like it may find their way into other procedures to help decrease the risk of Musculoskeletal disorders and injuries to users and provide safe and effective healthcare.